Psychiatry: Moving From Ice Pick Lobotomies and Chains Into a Brighter Future

This is a sketch of James (William?) Morris, an American sailor who was committed to London's Royal Bethlehem Hospital (Bedlam), an institution dedicated to the care of the mentally ill. The sketch was originally rendered in black and white by George Arnaud (1763-1841) and then rendered in color by George Cruikshank. According to Graphic Arts (publication of Princeton University), Norris was admitted to the hospital in 1800. He behaved so badly that he was chained and remained that way for years, as shown in the drawing. The picture is in the public domain because its copyright has expired.
Ten-year-old Giovanna M. had a really bad headache. She consulted a doctor. He admitted her to a hospital where it was determined she was mad. Three years later she was sent to Sant’Antonio Hospital, an institution devoted to the care of the insane. The record is sparse on the course of Giovanna's treatment, but certain facts can be ascertained. She was consigned to the basement of Sant’Antonio, where she was chained with others judged to be mad. According to Giovanna's description, fifty people were confined in the basement, and these lived in their own excrement while rats gnawed on their open sores. At some point Giovanna was transferred to another hospital. She spent an indeterminate period of time there, but was eventually sent to Villa Clara, which was another institution devoted to the care of the insane. At Villa Clara she received the most "advanced psychiatric therapy", which included purges, tonics and insulin.
Finally, at the age of ninety, Giovanna was released: she passed away. She herself remarked that fate did not grant her the mercy of an earlier death. Her parting assessment: "Eighty years in a psychiatric hospital for a headache."(From Clinical Practice in Epidemiology in Mental Health).
Civil Hospital San Giovanni di Dio, Cagliari, where Giovanna spent time before she was transferred to Villa Clara. Image credit: Cristiano Cani. The photo is used under a Creative Commons-Attribution Share Alike 2.0 Generic license.
Unfortunately, in the annals of psychiatry, Giovanna's history is not extraordinary. This is a profession that no doubt has had many compassionate practitioners who strove to relieve suffering. However, with little understanding of the underlying causes of mental illness, these practitioners more often than not missed their mark. Today there is a movement afoot in psychiatry to bring clarity and an objective approach to the profession, by incorporating tools of hard science. This movement toward objective, evidence-based psychiatry has met resistance.
Throughout history, those suspected of being mentally ill have paid dearly for the lack of hard evidence to support their diagnoses. It was an awareness of this suffering that motivated one of psychiatry's severest and most capable critics, Thomas Szasz to do battle with the mainstream of his profession. Dr. Szasz once explained that, as a child, he realized there were two sorts of hospitals: hospitals people could get out of and hospitals people would never be able to leave. Dr. Szasz made it his mission in life to do away with the second sort of hospital--mental institutions. He wrote many books on this subject, one tellingly entitled, Coercion as a Cure: A Critical History of Psychiatry. Dr. Szasz believed that a diagnosis of insanity was merely a description of behavior that deviated from the norm. He did not believe deviation from the norm was a pathological condition, and he certainly did not believe that psychiatrists had the right to force a "cure" on anyone.
If we consider the record of psychiatry, we may find ourselves sympathetic to the Szasz perspective. With flimsy evidence, and often impelled by superstition, "healers" have imposed horrendous "cures" on countless patients over the centuries. Here I've listed a few of the more remarkable remedies. Each represented the wisdom of the medical community at the time.
Lobotomy
This photo shows a drill that used to perform lobotomies on people in Norway. The procedure, according to the picture's caption, was performed in that country between 1942 and 1955. Picture is credited to: Bjoertvedt and is used under a Creative Commons Attribution-Share Alike 4.0 International license.
This therapy has perhaps become more notorious in popular culture than any other psychiatric intervention. Most of us know that a lobotomy involves some sort of surgery on the frontal lobe of the brain. What may be surprising is that different doctors approached that operation in different ways. And lobotomies were not performed exclusively for psychiatric issues. The procedure received such general acceptance that it was used to treat back pain, arthritis and headaches.
The first lobotomy was performed by Antonio Egas Moniz, in Portugal. The year was 1935. For introducing this medical intervention, called at the time psychosurgery, Moniz won the Nobel Prize. The procedure, or some version of it, was performed on people of all ages. The youngest patient I came across in my reading was a twelve-year-old boy, Howard Dully. Although his personal physician judged the boy to be fine, his stepmother complained about his behavior. His bad acts included fighting with his brother, disobeying his parents and taking sweets without permission. The stepmother consulted Dr Walter Freeman, who thought a lobotomy was justified, and accordingly, in 1960, performed his famous "ice pick" procedure. Years later, Dully, in an interview with The Guardian, described feeling a sense of loss when he thought about his lobotomy, "like you've lost a whole part of your life".
Amazingly, lobotomies are still performed today in the United States, although the procedure is now called a cingulotomy,.
Insulin Shock Therapy
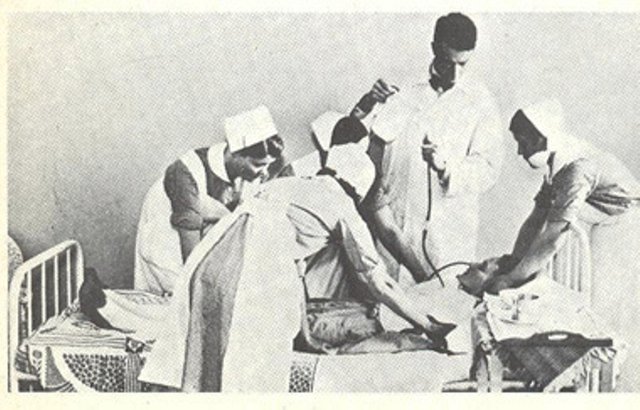
The caption under this picture explains that an insulin-induced coma is terminated by the introduction of glucose through a "gavage" tube. The scene shown in the photo took place in the 1950s, in a Helsinki hospital. The image is in the public domain.
It was an Austrian , Manfred Salek who came up with the idea of insulin shock therapy. In 1933 Salek started to use insulin-induced comas to treat schizophrenia. The course of treatment could include as many as sixty induced comas. Each of these insulin comas lasted about three hours and was reversed with the introduction of IV glucose. The practice was widely accepted in Western countries for about twenty years. It was eventually discredited, particularly after a controlled study in 1962 showed the treatment to be ineffective. Eventually, some analysts theorized that the calming effect patients seemed to experience after the course of treatment may have come from brain damage suffered during the coma. Estimates of mortality from the procedure vary. Once source suggests a mortality rate between 1 and 4%.
Trepanation
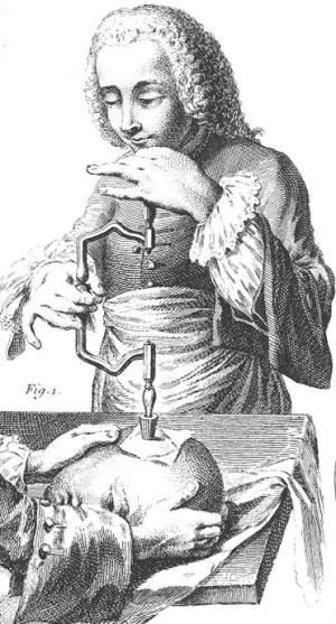
This illustration of a trepanation is from eighteenth-century France. The author is unknown, and the image is in the public domain because the copyright has expired.
Trepanation involves cutting holes in the skull. This procedure should not be confused with lobotomy. Lobotomy involves cutting into the brain and excising tissue or merely scrambling part of the frontal lobe.
Trepanation is an ancient practice used to treat both physical maladies and mental illness. In the case of mental illness, the logic of the treatment was clear. Demons possessed the mad. By drilling a hole in the skull the demons could be released and the patient cured. Trepanation was a widely performed procedure that many people survived. It is not known how many eventually succumbed to the effects of the surgery.
The Swing Chair

A 1792 portrait of Erasmus Darwin by Joseph Wright. Public domain image, expired copyright.
This invention was not in particularly widespread use, but it is included here as an illustration of how the supposed insane were powerless before the ingenuity of their keepers. The swing chair was the brainchild of Erasmus Darwin, Charles Darwin's grandfather. This distinguished physician noted that children were calmed when they played on a swing. So, he devised a box, open on one side, in which patients would be strapped and then twirled with such rapidity that they would experience vertigo, vomit and often lose their bowels. Patients subject to this 'treatment' were reported to show an improvement in behavior--it has been suggested that the improvement may have been due to apprehension about being subject to the "cure" once again.
The Triad of Twentieth-Century Psychiatry:
Psychoanalysis, Nosology, and Pharmacology
Together, these three tools have constituted the pillars of modern psychiatric practice, at least up until now. Each one of these pillars has played a critical role in psychiatry--although one of them, psychoanalysis, has fallen into less favor in recent years. Generally, a psychiatrist will use a combination of the three: symptom observation (nosology), talk (psychoanalysis) and drugs (pharmacology).
The three pillars, considered separately:
Probably the two most culturally influential figures of the twentieth century were Albert Einstein (Theory of Relativity) and Sigmund Freud (Psychoanalytic Theory). Einstein altered the way we regard the physical universe and Freud altered the way we regard ourselves. The first realm is the concern of physicists, the second the concern of psychiatrists.

This photo of Sigmund Freud was taken in 1920. The photo was shot by Max Halberstadt (1882-1940). The image is in the public domain because its copyright has expired.
Freud's effect on the practice of psychiatry in the twentieth century, and even today, cannot be overstated. Bertram Brown, one-time head of the United States National Institutes of Mental Health, once explained that for a time it was "almost impossible" in the US for someone to hold a chair or become a professor in an academic department of psychiatry unless they followed a psychoanalytic model in clinical practice. This psycho/social orientation--that is, viewing mental illness as a function of personal history and social context--led psychiatrists away from a biological consideration of mental illness. Psychosis was not a disease of the brain or body, it was a disorder of the psyche that could be rooted out by psychoanalysis--'talk therapy'.
II. Nosology
This refers to the effort, begun after WWII, to systematize the practice of psychiatry. The systematization began with the collection of data and grew to be a compilation of two massive diagnostic manuals--one, the ICD, issued by World Health Organization and the other, the DSM, issued by the American Psychiatric Association. Though the manuals were not identical they were periodically revised and there was an effort to reconcile them with each new edition.

This is the cover of a document prepared by the U.S. government that attempts to catalogue symptoms experienced by veterans of the Gulf War. It is the science of nosology which enables this sort of classification. While this document is neither the DSM nor the ICD, it does utilize the same methodology for diagnosis and treatment of illness. Since the image was produced by a U.S. government employee, the picture is in the public domain.
So far, since WWII, there have been five versions of the ICD and five versions of the DSM. In the most recent versions, the goal has been to offer psychiatrists a kind of checklist of symptoms that would lead to diagnostic consistency. The art of categorizing illness is called nosology. While clinical practice for most psychiatrists is governed by the categories described in the ICD and the DSM, a growing chorus of dissent has risen up from reputable quarters.
The three most serious criticisms lodged against traditional psychiatric methods of diagnosis are: A. Lack of reliability;* B. *Pathologization of "normal" behavior; and C. *Focus on symptoms, rather than causes of a disorder*.
These controversies explained, briefly:
A. Reliability: the same patient can consult three different doctors and may come away with three different diagnoses. The criteria from which the psychiatrists work, derived from the DSM (in the U.S.), are dependent on subjective impression and variability of patient presentation.
B. Pathologization: The sheer proliferation of categories has led to increased diagnoses, when many behaviors described as disorders are actually normal reactions to circumstances. Grief is one example often given to illustrate this point. The question is asked, how is a "normal", reasonable, response to loss distinguished from a pathological depression?
C. Separation from Causation: This last criticism is having the most profound effect on the direction of psychiatry today. Many critics point out that every other medical specialty supports diagnosis and treatment with concrete evidence--blood tests, computer imaging, genetic markers. Only in the DSM, the diagnostic bible for psychiatrists in the U.S., is evaluation and treatment prescribed based on a collection of symptoms alone.
This picture, by Craig Finn, shows what it feels like to have schizophrenia. Mr. Finn was reflecting his own perception of the world, as a patient who was being treated for the disorder. This remarkable picture was released into the public domain by Mr. Finn.
III Pharmacology
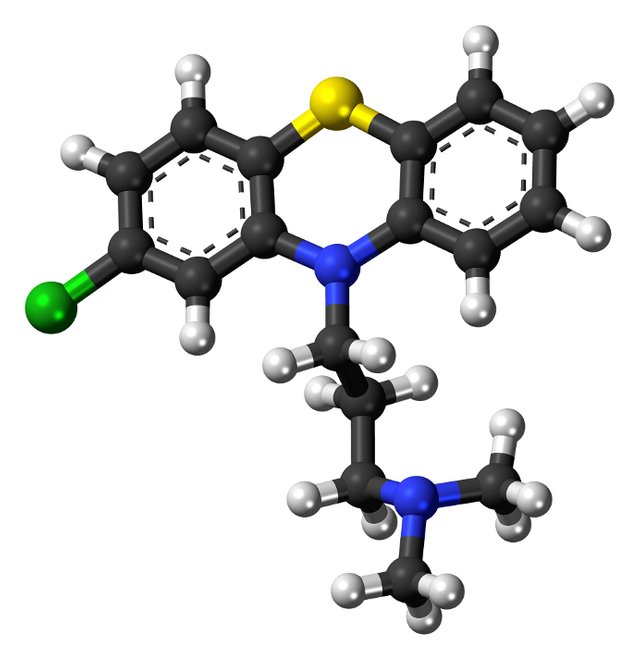
This is a model of a chloropromazine molecule. It is color coded: Carbon (C) -- black; Hydrogen (H)--white; Nitrogen (N)--blue; Sulphur (S)--yellow; Chlorine )Cl--green. The image has been released into the public domain by its author, Jynto.
In 1952 a drug called Chloropromazine went on the market in France. Its effect on the behavior of the recalcitrant mentally ill was obvious. People were calmed. Wards became quiet. This drug set psychiatry on a new path: psychopharmacology.. While the active mechanism for chloropromazine was understood (it blocked dopamine receptors in the brain) in most cases no one understood the way in which some of the other pharmaceuticals worked, though they did seem to work. The assessment of efficacy came from the fact that the behavior of some psychiatric patients, under influence of the drugs, was altered.
This image of a patient bound in an actual straight jacket comes from the Wellcome Trust.. The Trust is a repository of images that it offers freely if proper attribution is given. This drawing is used under a Creative Commons Attribution-Share Alike 4.0 International license.
Over time, however, psychopharmaceuticals came under attack. Chloropromazine (better known as Thorazine), for example, gained a reputation for being a chemical straight jacket because of the numbing effect it had on patients. There were other reasons for the decline of this drug's popularity. It was discovered that serious, irreversible side effects could and did ensue from its use.
Unlike chloropromazine, some of the other antipsychotic drugs are prescribed without an understanding of the mechanism that leads to behavior modification. Two of the more commonly used are haloperidol and perphenazine. According to the description of haloperidol on Science Direct the " The precise mechanism of action is unclear". A similar description of perphenazine is found on DrugLib, which states "the site and mechanism of action of therapeutic effect are not known."
A Break with the Past: Biological Psychiatry, Neuropsychiatry
PET Scan
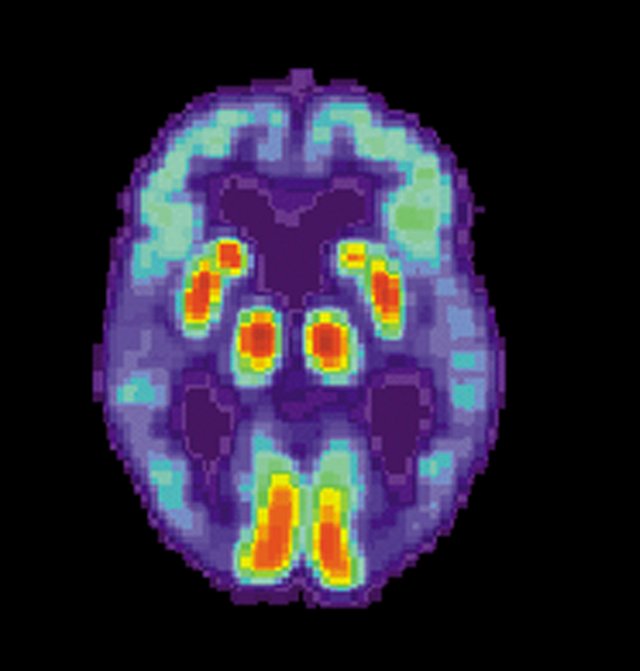
This image shows the PET scan of a patient with Alzheimer's Disease. The image was made by the U.S. government National Institute on Aging and is in the public domain.
In 2009, Paul R. McHugh, former Director of the Department of Psychiatry at Johns Hopkins Medical School, wrote an essay, Psychiatry at Stalemate, in which he took a sober look at the history and direction his profession had taken. It would be hard to find a more establishment figure in the field of psychiatry than Dr. McHugh. His assessment that psychiatry was in need of reform was all the more persuasive because of his stature. He points out something that is obvious to a lay observer: psychiatry treats symptoms but not causes. He explains that the "generative" nature of a disorder is not addressed in a course of treatment, just its expression. He asks, in his essay, what a patient is to make of a diagnosis that fits "criteria" for a disorder? Should the patient believe he is afflicted with a disease? Or is the difficulty the expression of an emotional state? In pinpointing psychiatry's lack of diagnostic clarity, Dr. McHugh highlights the major target of reformers in the profession. Although, to be sure, not all clinicians believe reform is called for. However, those that do want reform strive to bring psychiatry into line with the diagnostic methodology employed by other medical specialties.
Another influential voice for reform is Dr. Thomas Insel, previously Director of the US National Institute of Mental Health (NIMH). The NIMH is about as mainstream as you can get. Yet, when the most recent DSM was released, DSM5, in 2013, Dr. Insel expressed strong reservations. These reservations placed him at odds with establishment views. Dr. Insel explained that psychiatry does not do patients a service by focusing on symptoms which are entirely dependent on subjective reporting and observations. This diagnostic method is not reliable, in Dr. Insel's view, because it is not supported by physical evidence, or biological data.
This photo of Pilgrim State Hospital in Brentwood, New York, was taken in 1941. The hospital was designed as mental health facility, for the care and confinement of the mentally ill. Today, most of Pilgrim's grounds are closed, although part of the facility still treats patients. This image is from the Library of Congress, and according to the Library's records, the picture it is in the public domain.
Dr. Insel explained in a recent interview that without biomarkers, psychiatry lacks objective validity. The DSM, as it is now constituted, is merely a consensus document. In order to compile the manual, psychiatrists vote on what they think should be included and how it should be categorized. This becomes as much a political compromise as a medical guide.
Both Dr. Insel and Dr. McHugh, to varying degrees, address an issue that is the focus of a new sort of psychiatry. Called biological psychiatry, or neuropsychiatry, it involves a transdiagnostic approach. This incorporates traditional subjective factors with objective indicators such as computer modelling, "physical disturbances"(for example EEG results), and biomarkers (for example, indications of inflammation).
A researcher in the vanguard of neuropsychiatry, Daniel S. Barron, who holds both an MD degree from Yale and a PhD degree in brain imaging from the University of Texas, articulates the inevitability of wedding brain research to traditional psychiatric tools. Dr. Barron explains how knowing a patient's "neural hardware" can lead to understanding the underlying cause of symptoms and thus enable targeted treatment. He draws a comparison to another scenario, a patient with chest pain in an emergency room. The symptom of chest pain raises any number of possibilities. Medical history, social context (what were you doing when it started, for example), chest imaging and blood work are all helpful in arriving at a reliable diagnosis. It would be absurd to think the data derived from blood work, imaging and other objective tests were not essential to this procedure.
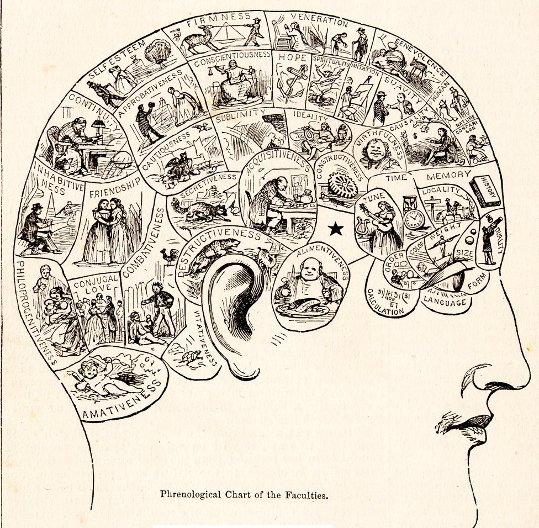
Phrenology was a "science" that was supposed to inform doctors about the human psyche. The shape and size of the skull were believe to reveal something about the character and personality of an individual. This image is in the public domain because its copyright has expired.
In a way, the new wave of psychiatry, which utilizes objective data to drive treatment and diagnosis, is a repudiation of all the horrors of psychiatry outlined in the first section of this essay. Early practitioners had no understanding of the physical basis of behavior. Their goal was to tamp down troublesome symptoms, at any cost. A cure was not a cure, but merely compliance. A lobotomy, Thorazine, and insulin shock may have had the effect of making patients more docile, but usually these treatments were at great cost to the patient and often the "cure" was not of long duration.
There are voices that caution against moving too quickly. The future of psychiatry as a science and branch of medicine is evolving. It behooves those of us who are not in the profession to pay attention, since some form of mental illness is likely to touch our lives, either directly or indirectly.
Some Sources Used in Writing This Blog
https://www.princeton.edu/~graphicarts/2010/01/an_insane_american.html
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3480686/
https://www.syracuse.com/news/index.ssf/2012/09/dr_thomas_szasz_critics_discus.html
http://www.centerforindependentthought.org/coercion_as_cure.html
https://listverse.com/2009/06/24/top-10-fascinating-and-notable-lobotomies/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4291941/
https://www.theguardian.com/science/2008/jan/13/neuroscience.medicalscience
https://www.medicalbag.com/despicable-doctors/walter-freeman-the-father-of-the-lobotomy/article/472966/
https://dublin.sciencegallery.com/failbetter/icepicklobotomy/
http://modernnotion.com/history-of-lobotomy/
https://www.britannica.com/biography/Manfred-J-Sakel
https://www.ncbi.nlm.nih.gov/pubmed/13859190
http://frontierpsychiatrist.co.uk/things-that-have-given-psychiatry-a-bad-name-2-insulin-coma-therapy/
https://www.tititudorancea.com/z/insulin_shock_therapy_58.htm
http://home.wlu.edu/~lubint/touchstone/2000/Trephination-Chew.htm
https://www.cvltnation.com/horrifying-psychiatric-treatments-from-the-age-of-reason/
http://www.ucmp.berkeley.edu/history/Edarwin.html
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2783473/
https://www.simplypsychology.org/psychoanalysis.html
https://www.mind.org.uk/information-support/drugs-and-treatments/antipsychotics/
https://www.amnh.org/exhibitions/einstein/einstein-s-revolution/
https://www.dw.com/en/freuds-pivotal-role-in-understanding-the-mind/a-1992871
https://www.nimh.nih.gov/about/directors/index.shtml
https://pdfs.semanticscholar.org/a544/53fa8ce0083c9c4a4aaf89ade3bd13b0251f.pdf
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2783473/
https://www.psychiatry.org/psychiatrists/practice/dsm/history-of-the-dsm
https://www.medscape.org/viewarticle/436403
https://blogs.cdc.gov/inside-nchs/2013/04/18/nosologists-what-do-they-do-and-why-is-it-important/
https://www.ncbi.nlm.nih.gov/pubmed/26098046
https://www.ncbi.nlm.nih.gov/pubmed/24470508
https://www.nimh.nih.gov/about/directors/thomas-insel/blog/2013/transforming-diagnosis.shtml
https://www.mind.org.uk/information-support/drugs-and-treatments/antipsychotics/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2655089/
https://www.ascpp.org/resources/information-for-patients/what-is-psychopharmacology/
https://www.coursehero.com/file/p6ku5tq/15-What-is-a-chemical-straitjacket-Chlorpromazine-Thorazine-was-the-first-and/
https://www.medicinenet.com/chlorpromazine_tablets_liquid-oral/article.htm
https://www.sciencedirect.com/topics/neuroscience/haloperidol
http://www.druglib.com/druginfo/perphenazine/description_pharmacology/
http://www.dana.org/People/Authors.aspx?id=37752
http://www.dana.org/Cerebrum/2009/Updating_the_Diagnostic_and_Statistical_Manual_of_Mental_Disorders/
http://healthland.time.com/2013/05/07/as-psychiatry-introduces-dsm-5-research-abandons-it/
https://www.medscape.com/viewarticle/892473
https://www.biologicalpsychiatryjournal.com/
http://www.psychiatrictimes.com/neuropsychiatry
https://onlinelibrary.wiley.com/doi/full/10.1002/wps.20514
https://medicine.yale.edu/psychiatry/education/residency/about/daniel_s_barron.profile
https://blogs.scientificamerican.com/guest-blog/why-psychiatry-needs-neuroscience/
https://www.nytimes.com/2016/10/15/opinion/theres-such-a-thing-as-too-much-neuroscience.html
https://www.nami.org/Learn-More/Mental-Health-By-the-Numbers





What a well researched article that is. It must have taken hours and hours of preparing it. From the over all reading I derive that one always should be critical about treatment, whether it's physically or psychologically.
What will people say in a hundred years ahead about the current treatments?
I am not a friend of generalisations and I think that every person should be regarded and treated unparalleled.
Are you familiar with Systemics?
In case of abnormal behavior it is always interesting to see how normal the surrounding system actually behaves. I tend to see people's craziness as a logical consequence of what they perceive and express as disturbing in the system. When someone is mad, he also reflects the madness of those around him.
The more compulsive the influencing systems, the more compulsive the individual human being.
Since the scale is wide and the expressions are strong or less strong, only those that are more extreme than the others stand out.
How is anyone supposed to go that crazy if there have not been causes that have led to this madness and that cannot be attributed to influential systems?
I therefore see madness more as an indicator of normality and the will to express oneself. People start to bother themselves and others because something doesn't seem right.
If I assume that disruptive behavior points to a resource and it is not considered scary and to be eliminated, then there is much more hope for healing than if I am afraid of a madman and want to sedate him.
Our biggest problem with disorders is that we want them gone too quickly and have neither time nor patience to accompany a slow healing process.
It would also be worth emphasising the acceptance that some people might actually be mentally ill and untreatable. I think that our modernity is obsessed with improving everything and thinking that, in principle, illness can always be cured and death defeated. I think that is questionable.
I don't know Systemics, but war and famine came to mind. What might be out of order in better times becomes "normal" in other times. However, I think we need to look at the brain, at circuitry, for the source of some mental disease. Because I do believe there is mental disease, where people suffer. There may be inflammation or trauma, or any other reason. The disease could be treated if we understood the physical basis. I have a brother who suffered a bout of autoimmune encephalitis. At first it seemed he had dementia, then blood tests revealed physical abnormalities and treatment (mostly immune suppressants) stopped the inflammation. Not soon enough to prevent all damage, but at least the treatment brought him back. I think that is an example of how understanding the physiology of brain disease (that's how I see mental illness) will help to alleviate suffering. For me, that is the point of all medicine.
Thank you for your kind words. It did take many hours. I usually approach subjects I'd like to learn about. I keep reading and then write. It's not an efficient way to proceed, but I learn a lot :)
I understand. It's important to talk about personal cases. What you tell about your brother, makes sense. If there are cures which help the suffering and the surrounding family members they should be sought. I also believe that there is mental illness. I've seen it many times. I am having the view that people could be less afraid of them and handle illnesses more calm. I am against pittying people and instead look for remaining resources and strength in both, the patients and the people around.
So much work on a serious part of medicine history and so less people interested. Perhaps they don't want to hear about it. I - for example - could not read the part in the middle of your post - it is like horror to me!
Why didn't you divide your post into two or three parts? Perhaps you will get more readers then? It is full of informations - so that can be done "easily".
Thank you @kadna! I should break it up. I thought about doing that, but the old teacher in me couldn't let go. I had to make my case. I had to let people know what I had learned. Efficiency is not my strong suit.
As you can see from the references, most of the information was new to me, also. Trimming, editing, that's the hard part. Learning is the best part. Thank you so much for your support. I can't promise to write less in the future, but I will try :)
I remember you told the same before. Make peace with your inner teacher - he is not wrong but his time is gone. Nowadays people are used to get information like fingerfood - part for part, step by step and not so much at the same time. So - you need not to make 10 parts ;-) but 2 or 3 and everyone will wai for the next part to continue the knowledge... You have enough informations for many posts! Yopur inner teacher has to see and believe that and he will be proud of you next time hihihi. Give it a try!
I have my next thought for a blog. As I write, I will keep your wise advice in mind. Plan it, perhaps, in several parts. So much research goes into the blog-- I ought to really get more mileage out of it. Perhaps the teacher should retire, and let the writer take over :)
Yesss - so show him that you are able to...;-) Hihi good idea.
:)
It's a pity that a post well documented and rich in historical and scientific information like this is nearly unnoticed and poorly upvoted. I resteemed it, because Steemit needs more of these thoughtful contents.
Also, tip!
Psychiatric hospitals are "total institutions", like jails, and innumerable violations of human rights were committed in them, up to the work of enlightened people like Erving Goffman in the USA, Michel Foucault in France or, here in Italy, Dr. Franco Basaglia.
Thank you for the feedback and the references. I did a lot of work, and tried to do justice to the topic. Many enlightened pioneers no doubt overlooked. But I will find out about the pioneers you reference. This is a topic I may address again as time passes.
Thank you for the "tip". Much, much appreciated.
Congratulations @agmoore, your post has been selected by the @asapers for a resteem and a feature in our brand new curation post. Issue 79
What does this mean for you? Well first an upvote from some members of the team, we are no @curie or @ocd but who is going to be unhappy with some extra upvotes. Also each post featured in the article will receive a 10% share of the SBD generated from the curation post.
Keep up the great work and please consider supporting the @asapers with an upvote and/or a resteem on the post you feature in. Please wait seven to ten days for payout.
Your friendly @asapers
Giving back A.S.A.P
P.S. What a well written and researched piece of writing, thanks for the scary reminder of what a good age I live in. @insideoutlet
Great - this is really a well researched and interesting post!!!!! Have a look at @agmoore in the future ;-)
:)
Thank you @asapers!
Yeah... some of this was kind of distressing to read. It was hard to get Giovanna out of my mind. Such a tragic life.
Wow. What an undervalued article. I'm glad you commented on my post, as it brought me here and I have a new person to follow. I'm impressed with the amount of research that you put into this. Well done.
Thank you! I love research and writing. And I was really appalled by what I learned about the history of psychiatry. So I went at it.
These were some deeply disturbing part of the western medical, psychiatric, psychological and human history. It was as if as humanity itself had had a lobotomy.
So glad it is behind us now.
Well done, such an informative piece. Curation worthy for sure.
Thank you. Yes, disturbing. I think we all have a role to play in bringing change. We have to exert pressure so voices of reason prevail. I appreciate the support :)
Ahhhh, I remember you! I meant to come back for a longer visit, and didn't come around to it. You wrote the post on fossils. Another stellar piece.
You have a good voice, and beautiful narratives.
You are really kind....I work hard and it's nice that someone notices
And I hope you get more such notice and appreciation. ;)
Hi @agmoore! You have received 0.1 SBD tip from @marcoriccardi!
@tipU voting service | For investors.
That's astonishing. I guess the proponents of 'fasting for longevity' have got a point, assuming that's one of the things Giovanna had to undergo!
Overall a very fair (and readable, and really not at all as long as it looks) post.
I feel some of the criticisms directed against psychiatry could easily be directed against many branches or instances of regular medicine: treating symptoms rather than causes? Check! Without biomarkers psychiatry lacks objective validity? How about the fact that what's a normal level of x vitamin is determined by the mean in the population, and hence changes every decade? Sperm count is now much lower than it used to be, and the current normal value used to be considered low. All over the world sperm count is dropping, so the healthy level needs to be recalibrated. Obesity rises so the healthy weight value needs to be increased. Not to mention that each person is different and what's a high cholesterol level for one, might be a normal level for another. So I think medicine in general has a long way to go, not just psychiatry.
Well it depends. If it's Hachiko they raise a statue to it. If it's a modern person in Europe and he grieves the loss of his parent for longer than 3 months, he's given pills. Quite inconsistent. In one of Abigail's last posts I asked how a psychologist would treat a person who came in and was obsessed with his discovery that people can grow old, that they can become sick, and that they can die. I wondered if the psychologist would medicate the Buddha away. I think the person who thinks we should just accept sickness and death, is the really crazy person who should be hospitalized. The only sane ones in this case are the futurists: that's the proper response to those visions, and the only reason the Buddha didn't go there was because the option wasn't available to him.
Reading the (sad and extraordinary) article about Howard Dully, I wonder whether his young age was exactly the thing that saved him. At such a young age perhaps his brain was still plastic enough to heal itself, allowing him to circumnavigate some of the disability the operation might've caused.
PS: What's the asapers tag mean?
Well, first of all, you have to know you were partly responsible for this blog. I've been reading so many references because of your posts that I got caught up in the subject.
I agree medicine is culturally biased. It's just marginally better than psychiatry. One of my blogs, about diagnosing lupus, shows how subjective many branches of medicine can be.
I agree about Dully. However, what I didn't include ( how long can a blog be, after all) was that as a young man he was in and out of detention. Settled down later in life but early on had a hard time of it.
Thanks for the feedback and subjecting yourself to a long read. The blog took about a week to put together--so much information. I had to discipline myself. There was a time I was writing books, before Steemit. When I've found my stride here, I'll probably go back to it. I do love research and getting into a subject.
Rereading your comment--a part I didn't respond to: One of most influential writers of my youth was Miguel de Unamuno. If you are not familiar with him, he wrote a long, long essay called the Tragic Sense of Life(translated). He addresses your point, about the Buddha and awareness. While Unamuno is considered to be an existentialist, a "modern" thinker, he really starts at the same place that led to Buddha's awakening. I've no doubt many a psychiatrist would have viewed the despair of Unamuno and Buddha as pathological. But these men just had the courage to look into the abyss and come out with a way to go on.
I don't have great insight into "mental illness"--I do think throughout history it has mostly been normative, and also used for political and social coercion. But there are people tortured by a brain that is affected by a disease process. Right now we can't help those people, because we don't understand the process. Maybe the tools of science can change that.
I only know him by name; never read him. I'll check him out. 👍
Asapers is a curation project that tries to support undervalued posts. They spotted one of my posts a few months ago and I think they help bloggers to get a foothold. This is not a group with a lot of power--yet--but they definitely exude a positive tone. So I always include them. https://steemit.com/steemit/@hitmeasap/the-story-behind-project-asapers-and-why-i-decided-to-go-for-it
What a brilliant opening with Giovanna's story.
Gosh, the horrors that were considered treatment earlier make my skin crawl.
Super informative. While mental health and psychiatry are definitely evolving, more people are also finding the voices to explain what they feel. It's still difficult to trust medication, especially considering the horrible effects of the previously popular ones.
Thank you. Giovanna's story breaks your heart, doesn't it? Represents so much suffering by so many people. As far as being skeptical, I'm with you. It's very hard to trust life to the skill and ethics of someone else. And yet, from time to time, we must. Thanks for reading that very long post :)
resteemed this great work. Sic to see the parallel evolution. They used still hand drills (man with the hammer methods), when there was already kind of advanced pharmaceutics avaiable
Of all the scary things in the world, sometimes I think human beings are the most scary. The horrors we visit upon each other....it's mind boggling. Thanks for reading, resteeming and commenting. No horrors here :)