Are vaccines victims of their own success?

This is a going to be a post about vaccines, but has has no real need to be. At its heart we’ll be talking about risk, and how we think and act based on the perceptions that we form towards what is likely to cause harm. If you don’t like vaccines, that's fine, you could easily go through this post and exchange the word vaccine with the word seatbelt and the word disease with trauma from car crash, and it would largely get across the same concept.
As I’ve mentioned previously, I’m a psychologist that works in the field of vaccination. I don’t do any of that squidgy biology stuff to make the vaccines (although I do place trust in those that do), instead I look at public perceptions and beliefs towards the evidence based recommendations that are arrived at through the extent of their work.
Vaccine related risk judgements
Vaccines are a medical intervention. They are a tool that the public health system uses to prevent disease (yeah, so this is about the level of medical knowledge you’re going to get out of me in these posts). When thinking about vaccines we therefore think in terms of two interconnected beliefs, those related to the vaccine and those related to the disease the vaccine aims to prevent. Now, it is important to understand that these beliefs that we form are judgements of risk and nothing more. As I mentioned in my previous post, it is near impossible to stay up-to-date on 100% of the science out there on vaccination, there are certain tricks that we can use to remain as accurate as possible on our judgments (i.e. trust in a healthcare system), but no matter who we are we still make judgements.
Each of these risk judgments are made on two dimensions. Susceptibility, how likely we are to experience a negative outcome and severity, how dangerous it would be to experience a negative outcome. Each vaccine is likely to be judge differently based upon what judgements an individual holds related to the specific vaccine and disease.
Here are some of the beliefs that might be held based on differing judgments.
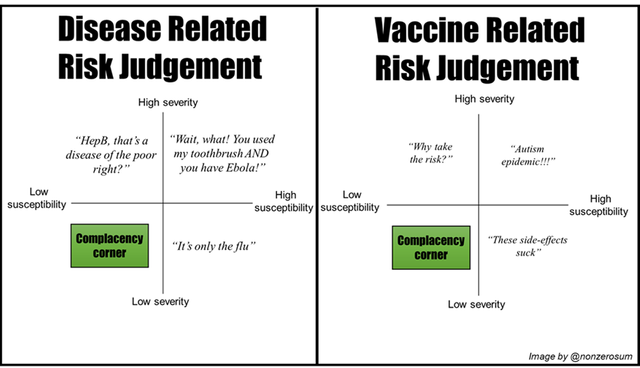
For each disease/vaccine pair we can imagine each of our beliefs being a point somewhere on each grid. The higher the perceived severity/susceptibility of side-effects from the vaccine, and the lower the perception of severity/susceptibility of the disease, the higher the likelihood of vaccine hesitancy.
If we apply this as a likelihood across to our grid it may look something like this:
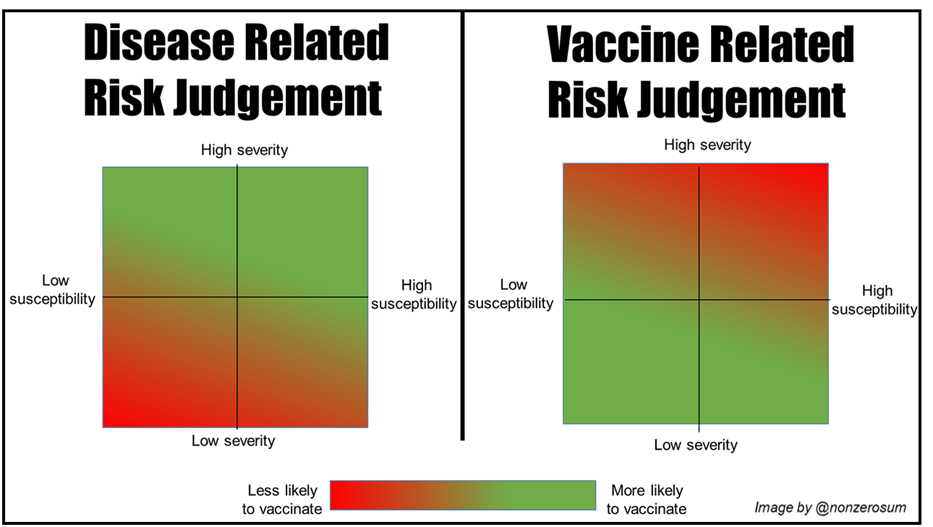
Place a point on each grid based on how you feel, combine the colours and compare it to the spectrum at the bottom and, job done, that's how likely you are to vaccinate.
Sadly not, there’s much more to risk perception than this, such as it being “fuzzy” and there being a difference between risk as analysis and risk as feeling. But for the time being let's just go with our simple model we have here and potentially revisit at a later time
Changes in risk judgements
Our perceptions of risk may change overtime through being exposed to new information. Information in this case might be statistical data related to how common a disease is in your local area, but it also might take the form of a story, such as that of a parent that believes their child's developmental disorder was caused by vaccination. The comprehension and processing this information may shift us in a certain direction on one of our grids.
A population wide example of this shift occurred in the winter of 2016 here in the UK due to two high profile cases of Meningitis B that became national news. At the time the MenB vaccine was only available (and cost-effective) for children up to the age of 6 months, the story of these two cases prompted a massive public demand for the vaccine to be made available for older children. Nothing had changed with respect to the diseases, it was still as prevalent and dangerous as ever however public perception of the disease had changed dramatically.
The introduction of an effective vaccine may change our perceptions in the opposite direction. As the prevalence of a disease reduces over the years our perception of susceptibility to the disease will, rightfully, reduce as a consequence.
This reduction of prevalence may have the additional consequence of less individuals within our local community contracting the disease and as such less stories being told about its severity. Take for example Polio, I’m willing to bet that many of you do not live in constant fear of you child spending their life paralyzed in an iron lung. In fact, in many countries the disease is fading from living memory entirely.
So wait a second, are you saying that people are right for not vaccinating?
Oh dear God no, this is what is so terrifying. One person not vaccinating, yes that's likely not going to have a massive effect, unless they travel to a country where the disease in question is still endemic. But hit a certain threshold of vaccine refusal and the the disease will bounce back and start causing mass suffering again.
This therefore is why in public health we often talk about vaccines being a victim of their own success.
The areas of the world with most hesitancy towards the vaccines are often the countries with the luxury of having low prevalence of disease. This safety becomes the new normal and the perception of threat may then move towards the vaccines instead.
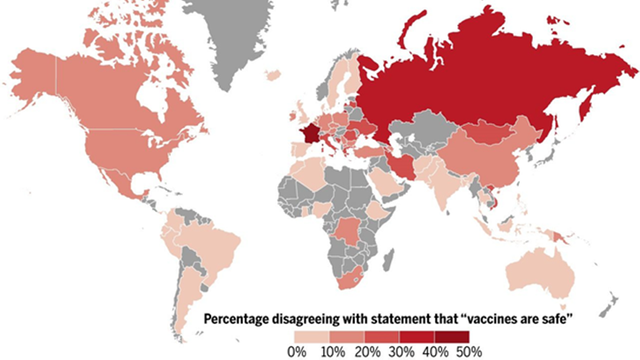
There is a cycle at play here that we are trying to prevent, one in which requires effective communication between a health system and the public. If we were to rely on fear to take hold for each disease before people rationalise to vaccinate, then untold preventable suffering would occur. Instead we need to find ways in which the importance of vaccination are communicated before the re-emerge of diseases.
Obviously there is much more to the vaccine decision making process than risk perception alone. In the next post in this series the plan is to talk about how this process of risk perception is applied to who, where and why we place our trust.
Sources:
Earle, T. C. (2010). Trust in risk management: a model‐based review of empirical research. Risk analysis, 30(4), 541-574.
Slovic, P., Finucane, M. L., Peters, E., & MacGregor, D. G. (2004). Risk as analysis and risk as feelings: Some thoughts about affect, reason, risk, and rationality. Risk analysis, 24(2), 311-322.
Reyna, V. F. (2012). Risk perception and communication in vaccination decisions: A fuzzy-trace theory approach. Vaccine, 30(25), 3790-3797.
The first inclination I had after reading your post was to mute you! Why you might ask. It is really simple and has to do with the reality of religions. As a deist I find it hard to listen to people who don't know the conventions of there own religion. Harder still is speaking to people who don't know they are practicing a religion.
The religion that is responsible for more crime and death all through history is called State ism. While most people who are members have good intention, they often do things that are morally reprehensible under the mistaken view that what they are doing will have some good effect that the world cannot do without.
The real problem with vaccines isn't that the idea is morally wrong. It is the practice of denying people a choice that is not only morally wrong, but also morally reprehensible. The cure is worst than the disease and the licensed professions involved are complicit in the crimes.
Indoctrination is also a disease that is promoted by the religion state ism. Of course I cannot prove that indoctrination causes the Dunning Kruger Effect, but the research I have done suggest strongly that is the case.
Even if I where able to prove it was the case do you think that the religion would stop the indoctrination? I strongly doubt that? There are however people who are a part of the heart and soul of the state ist religion that do think they would? So for me it is not that I hate the state, which would in my view be like getting made at Yogi the bear, but that from my own experience reality isn't part of the decision making process of state ist.
From my own experience most state ist don't have the power to distinguish the difference between a lie and simple truth. The heavy indoctrination somehow prevents the normal understanding that operating in truth is always better than operating in fraud. This truth cannot be taken out of the equation by more liars. The only solution is for the state ist to promote the truth, which is suicide for the state, and is why that is never going to happen. It is also why awake and aware people will never trust the religion.
Hi thank you for your comment. You're right within public health there is always a need to weigh up individual autonomy against protection of vulnerable individuals within the community. This is why your comment “The cure is worse than the disease” is so painful to hear, as it simply is not true. If vaccination were to stop tomorrow I am willing to bet that you would see evidence refuting your statement very soon after. To me the government's responsibility to the prevention of infectious diseases is similar to it's responsibility towards maintaining a clean water supply, whereby if they were to fail at their job there massive public outcry would be a very legitimate reaction.
I can understand why it looks like indoctrination from the outside, I clearly have a very different view of the government's role in society to you. So yes you may want to go with your first inclination and mute me as I'm likely going to post similar content in the future. Alternatively, you could follow me and have some of you preconceptions challenged, your choice ;-)
Clearly I have already decided to have my perceptions challenged. Maybe you will have some of your preconceptions challenged. That is after all the spice of life.
P.S What you don't address in my comment that is most interesting in the ancient Chinese interpretation of the word interesting. Perhaps if we are to challenge each others perspective it might be a good idea to address claims we do not agree with as well as providing those points we think have value in our discussions.
"The cure is worse than the disease” is so painful to hear, as it simply is not true"
Instead of dismissing my value judgement upon the practice of using violence to force people to participate against there will, which is the criminal behavior I spoke about. Pleas show me how using violence is not unlawful or not illegal. Please no magical reasoning as I am not up to such a conversation.
I never thought about it this way:
4.Populations start to think the vaccines are not needed.
There seems to be small sporadic outbreaks of infectious diseases lately so I hope that step 5 never really takes hold.
To the question in your title, my Magic 8-Ball says:
Hi! I'm a bot, and this answer was posted automatically. Check this post out for more information.