Is It Normal To Experience "Visitation" From A Dead Loved One?

Introduction
Hallucinations and hallucinatory experiences are probably more common than people presume.
Many contemporary textbooks of psychology or psychiatry will mention the phenomenon of post bereavement hallucinatory experiences (PBHEs).
This is when someone has a hallucinatory experience after the loss of a loved one.
The small amount of research that does exist on PBHEs and indeed the research on similar experiences in the general population suggests a very high prevalence of them.
Not only that but these appear to be mostly non-pathological in nature - often they are comforting rather than distressing to the bereaved person.
I will be discussing this from a scientific and psychological standpoint but that is not to detract from those who may believe that these are actual examples of contact with the dead.
Whilst I will be describing them as hallucinatory experiences that is not to imply that I have any special understanding of the causation.
Right now the scientific paradigm does not accept life after death so that is how these matters are covered but I try to keep an open though skeptical mind about all things.
I think what is more important is how the experiencer interprets these experiences.
This is a long post so I have produced my usual summary at the end.
Scroll down to bottom for the "Conclusion and Summary" section to get the TLDR version.
Hallucinations Versus Hallucinatory Experiences
It is perhaps useful to begin by defining some of the terms used here:

Hallucination
In it's most basic definition a hallucination is a perception in the absence of an (external) stimulus which is qualitatively indistinguishable from reality.
So in simple terms it is a person sensing something without a direct cause (e.g. physical object) in their external environment. It cannot be distinguished from their normal experience of reality.
Pseudo Hallucinations
Technically if someone has a hallucinatory type experience but it is in some way distinguishable as not real or only semi-real then that is termed a pseudo hallucination.
The difference between the two is the presence of partial or complete insight into the "unreality" of the perception.
Illusion
Misperception or misinterpretation of a stimulus is termed an illusion.
This is the commonest of all these experiences and something that we are all prone too, particularly when we are deprived of full sensory information e.g. misperceiving things in the dark.
Quick Example
If you see a tiger in your living room (when there isn't one) and believe it to be a real tiger then that would be a visual hallucination.
If you see it but don't believe it is real then it is a pseudo-hallucination.
If you mistake a piece of furniture for a tiger in the dark that is an illusion.

Hallucinatory Experience?
Hallucinatory experience is a broader category that is used to encompass hallucinations, pseudo-hallucinations and illusions.
This term is used because there can be some descriptive overlap between the categories particularly when lay descriptions are being used.
It also reflects the fact that definitions can evolve over time and there are variations in the literature.
That makes it hard to distinguish between them in some of the studies and to be honest it is still not completely clear how important it is.
Some would debate the necessity and say it depends more on how people respond to the situation.
It is probably best to see all these experiences as being inter-related and on a spectrum.
Further even true hallucinations which are normally considered towards the more pathological end of the spectrum appear to commonly occur in healthy people.
Felt Presence
This is the sensation or "feeling" that a (normally deceased) person is present in some manner but not necessarily via a direct stimulus such as sight or sound.
As Castelnovo et al. discuss there is some debate of what exactly this constitutes in terms of definition:
"“Felt presence” is usually referred to as an illusion, although its clear phenomenological and neurobiological nature remains elusive and largely left to speculation."
I think we can consider it as at least being in the spectrum of hallucinatory experiences.
The Literature is Scant

Performing a search on Pubmed showed a total of 60 papers.
However after sifting through them I was only able to access about 10 studies from about a maximum of about 15 that seemed relevant.
Many did not appear to be relevant upon reading the abstracts.
Some seemed quite obscure and only very tangentially related, others were so obscure that they did not even have an abstract which would allow this kind of determination.
It would be interesting to revisit this topic once I have greater academic and library resources at hand.
Luckily one of these was a very useful review by Castelnovo et al [1] which I have used to help me compile this article and which you can download the PDF for here (for free).
One of the primary things that these authors mention is the relative scarcity of direct literature on the subject and that would be consistent with my experience!
Results and Findings
These are summarised using tables followed by discussion of the figures below:
Table B Prevalence of PBHEs in the General Population
Mean Prevalence of PBHEs in the General Population is about 18%
Table 1 (on page 268) by Castelnovo et al provides a fantastic summary of the largest studies in the general population unfortunately it is text heavy and too large to fit here.
I have therefore constructed my own table with some of the most pertinent information as follows.
| Year | Authors | Sample | Size | Symptom | Prevalence % |
|---|---|---|---|---|---|
| 1894 | Sidgwick | Gen Population | 17000 | Hallucinations | 10 |
| 1948 | West | Gen Population | 1519 | Hallucinations | 14 |
| 1973 | Kalish & Reynolds | Gen Population | 434 | Hallucinations & Felt Presence | 23-41 |
| 1974 | Palmer & Dennis | College Students | 300 | Hallucinations | 17 |
| 1987 | Greeley | Gen Population | 1445 | Hallucinations & Felt Presence | 25 |
| Mean | 17.8 |
Discussion of the Data in Table A
Research on this topic goes back to at least the late 19th century.
Sidgwick [2] carried out a (massive) study on 19,000 people in 1894 with the aim of ascertaining the prevalence of PBHEs in the general population.
I did manage to get hold of a copy of this study to read and I must admit it was quite hard to understand!
One would not expect 120 years to make such a huge difference in comprehension.
Sidgwick has the largest dataset the others vary between 300 and 1500 participants.
These are still quite large for this kind of research - small sample sizes are sadly a limitation in most psychological studies.

The Rates Vary
Sidgwick found a prevalence of PBHEs of about 10%.
Later research by others suggested much higher values.
Kalish and Reynolds suggested a rate between 23 and 41% - unfortunately they did not distinguish between dream experiences of deceased people and hallucinatory experiences so this should be taken in mind.
The more recent study by Greeley (1987) does not suffer this issue and gives a rate of about 25% which is surprisingly high in my opinion.
One must wonder whether the difference is due to some methodological difference or changing cultural attitudes.
Were people more conservative about revealing this information in the 19th century?
Further it would be interesting to see if the rate has gone up in the intervening 30 years since the most recent study (1987).
One should be aware that these studies do not specifically look at bereavement, only the experience of perceiving a deceased person.
Technically bereavement implies some kind of loss and seeing a dead person you don't know doesn't really fit with this.
Mean Rate
The mean figure which I have calculated here is a fairly crude measure as it does not take account of the different sample sizes of each study.
Since the largest study was conducted over 100 years ago I am not sure whether some kind of weighting would be appropriate either.
Attitudes and culture change significantly over time and I do not feel that giving greater weight to this admittedly massive study would help.
What would be more useful would be to get a similarly large modern study - I suspect the stigma of coming forward about anomalous experiences nowadays may be even less amongst the general population than the most recent study.
Interestingly the rates of these experiences are even higher amongst the widowed population:
Table B Prevalence of PBHEs In The Widowed
Mean Prevalence of PBHEs in the widowed population is about 60%
Table 2 by Castelnovo summarises the studies looking at this population but again this would not fit here.
I have constructed a similar simplified table with a little extra information (from the individual studies) which I thought was relevant:
| Year | Author | Sample | Size | Symptom | Prev. % |
|---|---|---|---|---|---|
| 1958 | Marris | Widows in Stepney, London | 72 | Halluc. & Felt Presence | 50 |
| 1971 | Rees | All Bereaved Mid-Wales Area | 293 | Halluc. & Felt Presence | 47 |
| 1985 | Olson | 2 Nursing Homes Asheville NC | 52 | Halluc. & Felt Presence | 61 |
| 1993 | Grimby | 50% Wid. Goteborg b. 1912 | 50 | Halluc. & Felt Presence | 82* |
| Mean | 60 |
Discussion of Widowed Results

Inconsistency in Original Table
I found some inconsistencies in the original Castelnovo et al. table as it pertains to the Grimby [3] data - in their version of the table it says a prevalence of both 30 and 50%.
I'm not sure where they get that from in the Grimby paper. Here is what I found on reviewing the paper:
"One month after bereavement, altogether 82% of the subjects (89% of the women and 57% of the men) reported hallucinations and/or illusions; 36 % of those affected experienced only one type of hallucination or illusion, 30% had 2 types, 12% had 3 and 2% had 4 or 5 types."
I don't know if I'm missing something but I think the figure that should be used here is 82%.
I have therefore used the 82% figure to calculate the mean across the studies of 60%.
Of particular note here are the very small sample sizes, most being less than 100.
The Rees Study [4] has the largest size at 293 subjects.
Despite this it is quite clear that the rate is considerably higher in this population.

It could be said that one would expect this as the spousal relationship would be one of the closest.
If there was anyone that would prompt such an experience more one would expect it to be a husband or wife.
Of interest is the possibility that some of these studies may be under-reporting the true prevalence.
Here is an interesting piece of information from the Grimby study [3] in 1993:
"Despite great care being taken to create confidence in the interview situation, only one subject, a female spiritist, spontaneously reported hallucinations, referring to the frequent “contacts she had with her dead husband”. Only after being informed about the commonness and normality of post-bereavement hallucinations and illusions did most of the other widows and widowers speak freely, expressing relief from thoughts that they “might become or be considered insane”.
This shows that even 25 years ago there was a degree of cultural fear about discussing such experiences.
Given the recent popularity of paranormal TV shows and such subjects in general people nowadays may be less fearful of being labelled insane.
It would certainly be interesting to see if modern studies would give even higher rates.
There are hints that in other (non-European) cultures there may be different prevalences:
"Some case reports suggested that PBHEs may be considered more favorably among some non-European cultures, especially among some ethnic minorities such as Hopi Indians (Matchett 1972; Shen, 1986). Support from this view also comes from Japan, where hallucinations are considered normal concomitants of bereavement. None of the bereaved people studied express worry over their sanity (Yamamoto et al., 1969). However, of 18 widows interviewed 90% reported feeling of the presence of the dead spouse, though none reported cultivation of the idea of the presence of the deceased."
Other Associated Findings
Here are some of the main points that stood out in relation to PBHEs and their associations:

Older People Seem to be Affected More
Several of the studies seem to show a higher prevalence in those over 60, although there seem to be some that are not consistent with this.
Further one must also consider potential confounding factors that might impact on this e.g. medications (older people take more and some may cause these experiences as side effects), sensory loss (which increases the risk of perceptual abnormalities and early dementia/cognitive impairment.
The Rees study (which is the largest widowed study) shows a double peak at ages 49 and 69:
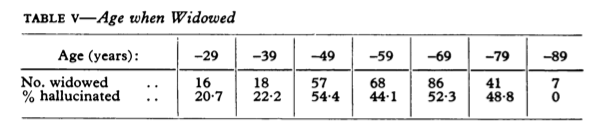

This is interesting and it is not entirely clear why this would be.
Anyway the age factor may directly tie into the next association too:
Women Seem to Have More PBHEs
This may be due to a direct relationship with gender or it may be due to the fact that women live longer on the whole.
For example in the Rees study there were considerably more women than men (226 F: 66 M) and this reflects fewer males in the potential population available to study.
This could serve to amplify any confounding factors due to the smaller relative population size of males.
As a further example if we look at the Olson study [5] which used a nursing home to do the investigation, the final sample consisted of 46 females to 6 males.
I think to truly distinguish sex differences (if they are present or not) it might make more sense to do a study on younger widows/widowers but obviously this presents problems in itself.
This is a substantially smaller population and there may be further issues with recruiting such individuals since earlier deaths are more likely to be from traumatic and un-natural causes.
There is also the understandable theory that death of any cause in a young spouse would be more unexpected and hence more traumatic - particularly if there are young children/family involved.
These people may be less willing to come forward and even when they do they may fear the consequences of reporting hallucinatory experiences particularly if they think it may result in their sanity and therefore their parenting being scrutinised.

Prevalence Increases With Emotional Attachment To The Deceased
This is not so surprising.
People who did not get on with their spouses are less likely to have hallucinatory experiences.
If one looks at this from a purely psychological perspective where these experiences could be considered an attempt by the mind to come to terms with the loss of a loved one then this makes sense.
If you didn't really love them, than there is no real need. You might actually benefit from the loss.
Those who believe in a more spiritual interpretation might also say this is in keeping with their beliefs - a true loved one is more likely to visit than someone you hated!
Note this wasn't explicitly examined in the general population studies so would be an interesting feature to explore in more depth.
Not Having Children Reduced the Rate of Hallucinations
This is interesting and may be part of the previous point.
It was primarily suggested by the Rees study.
Does having children increase the likelihood of having a stronger spousal bond?
Does this then lead to a greater probability of PBHEs?
Obviously not all families are cohesive and close so one would presume it does not always apply.
The Vast Majority of Experiences Are Pleasant/Comforting
In nearly all the cases covered in the widowed groups, the experiences are considered to be pleasant and comforting.
Negative experiences are rare. This would be consistent with PBHEs being some sort of psychological defence or means of dealing with the loss of a loved one.

Duration and Timing Varies
As Castelnovo et al point out:
"they can disappear shortly after mourning or persist for years, sometimes even for decades, usually occurring intermittently. Indeed, experiencing hallucinations and illusions was mostly reported to happen seldom or rather often (Grimby, 1993)."
It may be that certain subgroups are more likely to experience these types of phenomenon generally.
There does appear to be a pattern as it applies to those who have been widowed:
"Recurrent hallucinatory experiences seem most common in the early phases of bereavement, with a prevalence rate above 80% in elderly people within the first month of the loss (Grimby, 1993)."
"Stably high percentages of hallucinatory experiences taken as a whole have been observed during the first ten years of widowhood, followed by a trend toward reduction and disappearance with time (Rees, 1971)."
Timing throughout the day seems to vary in most cases but according to the Rees study there may be a minority of cases whether they only happen at fixed times of day or night.
This is interesting as one would expect more of these sorts of experiences to mostly happen at night - particularly if misperception is involved.
It is more common for people to experience "illusions" at night.
Just think of the situation of seeing a dark shadow a night and mistaking it for a sinister figure.
Factors That Don't Alter The Prevalence

Religion and Culture
None of the studies really suggested a difference being made by religious beliefs but one must consider the uniformity of the study populations here.
From my reading of the papers available to me the vast majority of subjects were Christians of a variety of denominations and it would be unlikely that their religious beliefs in regards to such experiences would differ.
I think of more relevance here would be to actually compare with studies such as the Japanese one by Yamamoto et al [6] mentioned earlier.
That one was performed in a population which is more accepting of such experiences.
Unfortunately most of the studies are in Western populations and the Yamamoto study had a tiny sample size of 20.
Geographical Factors and Education
Other factors such as geography and education did not seem to have any bearing on the prevalence either and we may again be seeing a uniformity effect in the populations considered.
If one considers western countries, then the educational disparities are significantly less than a developing country for example.
Similarly the differences between rural and urban communities will be much smaller in similar domains.
It would be interesting to test some of these factors in developing countries where superstition may be more common in rural areas versus urban settings.
Would there be a noticeable difference?
Other Limitations

I have already discussed the main limitations in the previous sections and to summarise they relate mainly to issues with sample sizes being small, over-representation of women and the cultural uniformity of the groups considered.
Another factor that I briefly covered is the distinction between what would be called true hallucinatory experiences and things like illusions and other perceptual abnormalities.
This is widely discussed in both the review and the individual papers but I think one could argue how important this is unless we are also simultaneously testing for mental illness.
The studies don't really control for pre-existing mental illness such as schizophrenia or psychotic depression where hallucinatory experiences may be present and hence confound the findings.
Without knowing this I am not sure what more we will gain from making the differentiation - since we will be unable to say if it is pathological or not.
This becomes a further problem in elderly populations where there may be undiagnosed dementia.
Certain types of dementia such as Lewy Body Dementia may cause visual (and other) types of hallucination.
Certain other conditions relating to impairment of hearing and sight (e.g. Charles Bonnet) may also result in abnormal experiences. As might individual strokes or epilepsy.
I also mentioned medication briefly earlier.
Another related issue to consider which I have come across myself (in elderly people as well as younger people) is alcohol and (perhaps a sign of the times) opiate withdrawal.
Both of these can cause hallucinations and should be taken into consideration.
Conclusion and Summary

Although there is considerable variation in the rates reported by different studies, it appears that post bereavement hallucinatory experiences are very common.
In the general population the rates vary between 10-25% (mean 17.8). In the widowed population the rates are considerably higher at 47-82% (mean 60).
There appear to be greater associations with female gender, increasing age and in the widowed population with the strength of the marital bond and having children.
Whilst these results are quite significant and point to high prevalences of these experiences within the populations studied they should be taken in context.
It should be noted that the research is generally quite old with the most recent studies being from the 1980s and 1990s.
The largest population based study is from 1894.
Multiple studies also cite the potential for under-reporting and it may well be that this has been modified in the decades since the last studies were carried out (in the 1990s).
There is also considerable variation in sample sizes and there may be uncontrolled confounding factors which may contribute to the differing rates shown.
Further gender differences may be accounted for by a lower frequency of men in the elderly populations studied and there may also be variation in reporting rates across studies depending on how the inquiry is made.
Of particular pertinence is the fact that none of the studies took significant measures to eliminate physical or mental health conditions which might predispose to hallucinatory experiences.
More research is needed to study larger populations and look in more depth at modifying and confounding factors.
It would also be useful to compare the rates in different cultures as most of the studies have looked solely at Western and European cultural populations.
A Japanese study from the 1960s suggests that the prevalence of such phenomenon in a culture that is more accepting of these experiences may be even higher (90%).
What we really need are contemporary large scale studies to look at these issues in more detail and establish how they fit into the context of mental and physical health.
Sadly this is not really a glamorous area of research so I am not sure if we will get that.
Anyway what do you think? Do you know someone who has had post bereavement hallucinatory experiences? Have you had them?
Let me know in the comments.
References
Castelnovo, Anna, Simone Cavallotti, Orsola Gambini, and Armando D’Agostino. 2015. “Post-Bereavement Hallucinatory Experiences: A Critical Overview of Population and Clinical Studies.” Journal of Affective Disorders 186 (November): 266–74.
Sidgwick, H., A. Johnson, F. W. H. Myers, F. Podmore, and E. M. Sidgwick. 1894. “Report on the Census of Hallucinations.” Proceedings of the Society of Psychical Research, 25–422.
Grimby, A. 1993. “Bereavement among Elderly People: Grief Reactions, Post-Bereavement Hallucinations and Quality of Life.” Acta Psychiatrica Scandinavica 87 (1): 72–80.
Dewi Rees, W. 1971. “The Hallucinations of Widowhood.” British Medical Journal 4 (5778): 37–41.
Olson, P. R., J. A. Suddeth, P. J. Peterson, and C. Egelhoff. 1985. “Hallucinations of Widowhood.” Journal of the American Geriatrics Society 33 (8): 543–47.
Joe Yamamoto, Keigo Okonogi, Tetsuya Iwasaki, and Saburo Yoshimura. 1969. “Mourning in Japan.” The American Journal of Psychiatry 125 (12): 1660–65.
Torrie, A. 1960. “Community Care of the Widow. A Social Service of Interest to the Family Physician.” British Medical Journal 1 (5181): 1267–70.
West, D. J. 1948. “A Mass Observation Questionnaire on Hallucinations.” The Journal of the American Society for Psychical Research 34 (644-645): 187–95.
“Hallucinations and Illusions.” 2017. Accessed February 18. http://www.priory.com/halluc.htm.
Thank you for reading

Before you go have you filled in the Coinbase form to list STEEM? It only takes a few seconds. THIS POST shows you how.
If you like my work please follow me and check out my blog - @thecryptofiend
Uncredited Images are taken from my personal Thinkstock Photography account. More information can be provided on request.
Are you new to Steemit and Looking for Answers? - Try:
Great article, cone again, and a special hat up for the level of respect and decorum taken throughout the article. This following part really underlined the openminded aspect of your article:
This is a subject very very close to me as I have been delving into the paranormal since I was born, in spite of myself... I have to admit that younger I wouldn't have been the sharpest of tool to know what may be what and wouldn't have been able to identify with an experience relating to a deceased person, especially if no imagery came through. The tools necessary to do so are much sharper now, luckily, and have had the chance of experiencing it twice. Mind you, though one can create a cut off for what is "reality" compared to what isn't, the legitimacy of it is extremely difficult to judge of without knowing how to access the same realm of experience. If two people had the same neurological predisposition and experiential baggage, maybe they'd have the same experience and be able to vouch for each other. From there, we'd need a third person to vouch for them and, if we weren't able to find the specific synchronous individual, the odds are that these two people would be deemed "abnormal" and maybe even a more debilitating label.
Corroboration of experiences that have a basis outside of conventional instrumental science doesn't get enough status for the validity of the experience. within the realm of the so-called social studies, there are mechanisms/methods that would allow for very decent studies of the matter though. The #1 problem becomes the one relating to the biases relating to the findings as well as what is implied in the conclusions from there. Rarely have I ever came across studies with an open end strictly conversing on the findings of what has been observed. You seem to have found a bit of a treasure trove in relation to that. Good for you good for us all! I greatly enjoy and value most of your discussion on the topic up above. Very well done, thank you.
From the stand point discussed up above, it is hard to know whether or not someone would trust another human being's judgement, as it is more often than otherwise the case, with such experiences. As you so well eloquently underlined, the cultural recognition or evaluation relating t such experiences could very well, and it would be my contention based on my experiences, that it would be the case. A general framework accompanying the study would have to be presented and understood first to be able to expose the potential relevance of such experiences within the frame of the social consciousness as well as within the mindset of each individual for that matter. Though the sharing of such experience is usually strictly forbidden within the cultures that have been practicing and and studying experiences of that nature, it might actually be a possibility, if one can gain trust, possibly after going through initiations and a longtime among the people...
If sincerely wish you good luck with this. Though we are now living in times where it seems apparent to you that the exposure of such experiences in the media might promote the ideas and concepts relating to such experiences, the war on consciousness is gaining in scale and, the heavy burdden left on the individuals exposing their views apparently countercurrent to the status quo as well as the apparently almighty mainstream of our Occidental white Englo-Saxon male culture, weigh very very heavily on one's sovereign soul-whenit is sovereign-, especially in times where that weight might simply not be welcomed.
Namaste :)
Thanks for such a fantastic answer. I think it is not just an issue of bias there is actual real fear of ridicule that stops people researching these things particularly those with more paranormal connotations. I think we might see things improve though.
I definitely agree with you, fear is a major issue on both sides of the equation and definitely underlines the lack of experience in relation to spirituality and the general level of consciousness around it.
What a great article it was. I went to bed still precessing the thoughts and even had dreams relating it, but that is a whole different ball game. ;) Namaste :)
Thank you, you are very kind. I love these topics and do hope we can reach a more enlightened state. True science does not ignore or fear subjects:)
Again and even more so now can only agree with you. Keeping the channels open for science and spirituality to work together only brings about a much wider understanding of the human realms as well as more potential pathways to enlightenment. Luckily there are already a few using science out in India, Tibet, Australia and so on. Seeing the merging of the two disciplines together through meditation and the study of quantum physics as well as neurology and many aspects of physics really opens up the field of potential. It is very exciting times! Namaste :)
Yes for sure!
I want to believe there is more after this that we are not totally gone. My gran who recently died promised me she would get in touch if she could, I'm still waiting and hoping she does.
Yes I remember you mentioned that. I think most of us exist in that hope.
What we need is more proof from the other side, A Skype connection would be good lol
There is lots and lots of proof.
But, americans are all programmed to think that it is just a few weird hallucinations, that aren't well documented, and definitely not peer reviewed.
But, this isn't the case. There are libraries of information on this. There are more reported incidents than you could read in a lifetime. The evidence is there if you look. Piles and piles of it.
However, this is a personal journey. You have free choice, so you can believe that the beings on the other side don't exist, and respecting your choice, they will never speak to you.
Almost any of the spiritual teaching paths will have you coming in direct contact, and from your personal experiences then you can find your proof.
And, the electronic device you asked for does exist. But, if you choose to not believe, all it will play for you is static.
I agree, I haven't had that luck byt would love to see someone, my father did, my grandad heard things that couldn't be explained so I'm open to it.
There is no proof strictly speaking I think you mean there is evidence. There is small amounts of evidence but it is inconclusive and not scientific. The big problem is funding and the fear of ridicule and that won't change until someone has the balls to take a chance and also put their money where their mouth is! If I ever become wealthy I will fund it myself because I find this kind of stuff fascinating.
My words I have used are very specific.
I could have written this post in my sleep, but today, you couldn't get me to write such even if you held a gun to my head.
The problem with science is that the current batch of potentates believe in a solid, atomistic universe. And anything that goes against that is called unscientific. Not that is unscientific, but that the potentates have declared it so. They would probably say love is an illusion, if so many people didn't feel it and know it.
As I have stated, I will restate. The amount of evidence is mountainous.
You have to look, wanting to see.
I think Thomas Edison did try that!
Very well written. I never before looked at studies on this but have read the criteria in DSM-5 for diagnosing it. It is interesting.
Thanks:)
Too bad they didn't distinguish dream. I've dreamt many times of people who pass away long time ago and have found others have the similar experience.
Me too. I still have dreams of one of my dead friends we are doing normal things like playing sports like football that we used to play.
I think some people would say it is a visitation of sorts.
Sometimes I even remember in the dream and say to him "Aren't you supposed to be dead?"
The weird thing is he just smile and changes the subject or something else happens.
Who knows for sure?
Yes that is a good question, there is a lot of literature on the matter but mostly from single sources and as stated above spiritists tend to share more of their experiences most people just sleep it off.
Yes - that is the problem with a lot of research. I am really interested in it but it doesn't do the subject any service if we accept weaker evidence as debunkers will destroy it.
Dreams are strange. Even years after graduating, I still dream of waking up late for going to the exam hall. Seems my friends also have similar dreams.
seems a bit hardwired that you have to get to those exams and do well or you aren't human are you from China by any chance I hear Asians get that from parenting also ups the IQ by about 10-15 points :D
No, I'm from Singapore but parents are stress over children's education here too.
Me too I am still having exam dreams!
Oh OK. So, it's seem not so culture drive. More global than I presumed.
I think we would need to see a study to be sure but it seems that way.
This logic is all fine and good, until it runs into reality.
If the dead person is really there and trying to make a connection, is calling this a mental disorder the best thing to do?
There are people who can plainly see the spirits and connections.
There are people that can hear and translate the messages from same spirits.
Of course you could disbelieve what is happening right before your eyes, but then, who is hallucinating?
And if you go to Tibet, and tried to talk about this article, they would smile politely and ask if you needed any help. (If they responded like americans, they would call you insane and throw you out)
That is your perspective perhaps.
It is not called a mental disorder. That is the point.
haha yeah :) probably well it's culture based yes. Westerners like to be in control, but they don't know the half of it. It's not that bad since people are open to the curiosity, it's just if you go into the crowd and say "I have a dream" and get shot :D figuratively speaking, sad part is it does happen from time to time.
I would like to read up on some material if you have any links to offer or ideas for that matter.