The xenobiotic metabolism: Your body’s daily fight with poisons.
The mechanisms of detoxifying the human organism involve different organs, enzymes and chemical reactions.
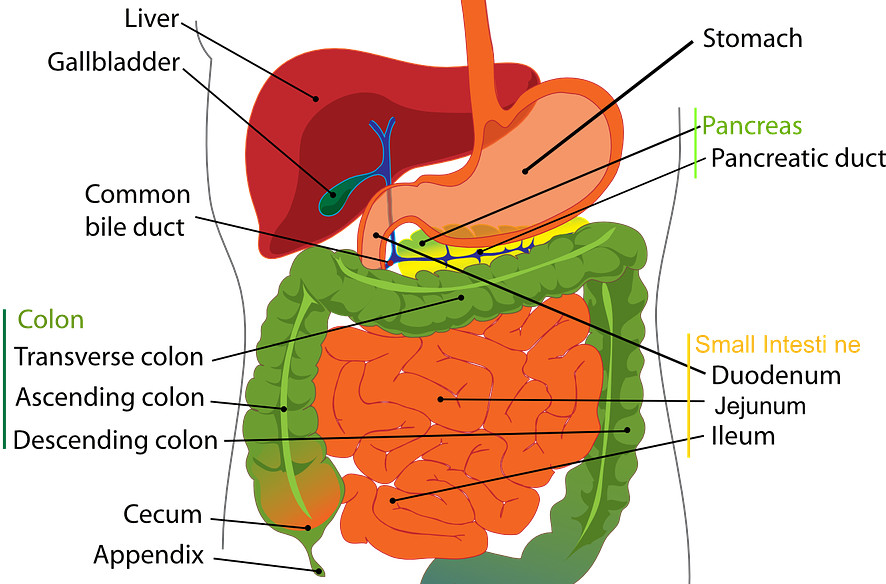 The liver - directly connected to the intestine via portal veins and bile duct - is main organ for metabolizing toxic compounds. Source: pixabay
The liver - directly connected to the intestine via portal veins and bile duct - is main organ for metabolizing toxic compounds. Source: pixabay
Intro
At all times the human body is exposed to foreign chemicals. They are in our food – derived from bith natural and artificial sources, but also in the water we drink and in the air we breathe, or we might take them as drugs. Many of those compounds are bioactive and/or toxic.
To survive this constant chemical storm, animals (including us) have developed a defence whose goal is to get rid of potentially dangerous foreign chemicals, the so-called xenobiotics (xeno=foreign, biotic=bio-active compound) by metabolizing and eliminating them. To understand the effect of a compound, you always have to understand its metabolism, which is therefore extremely important for both toxicological and pharmaceutical researchers.
Uptake and elimination
I will not go into detail on the different mechanisms at work here, as this would fill another post (some time maybe?). It should be said that uptake can happen via different organs, like the lungs, skin or different mucosa. But for now, let’s focus on the most important one: the intestine, or more specifically the colon.
As there are no active transport mechanisms for foreign chemicals, they have to diffuse through the cells of the gastrointestinal barrier in order to reach our blood stream. Cell membranes mainly consist of lipids. So to cross them, a compound needs to be quite lipophilic (“fat-loving”, i.e. it solves well in fat).
That’s the main takeaway here: the more lipophilic a compound is, the better the uptake. Thus, while hydrophilic (“water-loving”) xenobiotics are not taken up very well and quickly excreted, lipophilic chemicals enter the portal veins that transport nutrients from the intestine to the liver and consequently deliver them to the blood circle that distributes them over the whole body.
Our body has two systems for cleaning unwanted compounds from the blood: the bile and the kidneys. The former is a secrete directly produced by the liver, the latter are organs filtering the blood. Both have a common problem: only hydrophilic compounds can be excreted. So without further modification, lipophilic xenobiotics would accumulate in our system and reach dangerous concentrations.
The goal of the xenobiotic metabolism is to make those compounds more soluble in water, so that bile and kidney are able to sort them out. This process is one of the main responsibilities of the liver.
a scematic view of the liver - yes, again! An overstatement? I think not. Source: pixabay
The metabolism: Phase 1 – Functionalization
In the first phase, the taken up compounds are functionalized. That means – chemically spoken – that enzymes are used to add functional groups to the molecules in order to make them susceptible for conjugation (read below: phase 2).
The most important group of enzymes involved are “cytochrome P450”-carrying monooxigenases. They use their iron-containing core structure to catalyze the incorporation of an oxygen – in form of either a hydroxyl or an epoxide - into the target molecule.
Another phase 1 enzyme is the alcohol dehydrogenase – important for anyone drinking alcohol, as it catalyzes the oxidation of an alcohol to an aldehyde, which is then further metabolized to a carbonic acid (in case of “the” alcohol, ethanol, that’s first acetaldehyde and then acetic acid). Other enzymes add amino groups or reduce hydrocarbons.
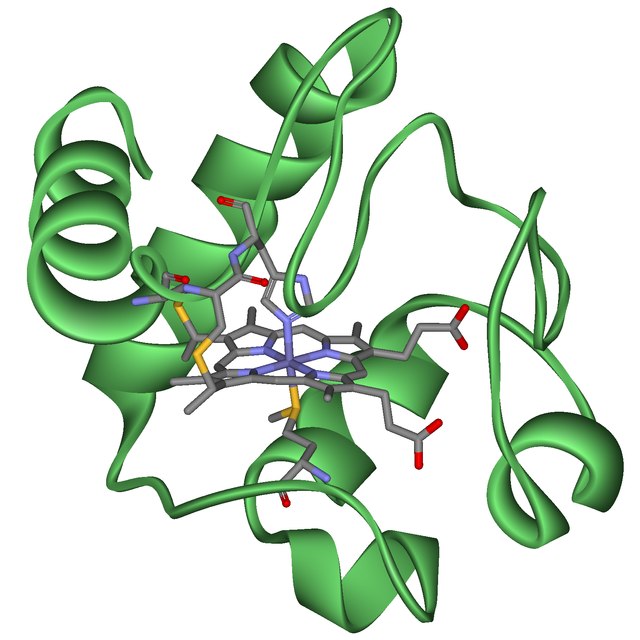 The iron-containing heme-structure is not only part of hemoglobin, but also the active center of metabolic enzymes. Source: Wiki.
The iron-containing heme-structure is not only part of hemoglobin, but also the active center of metabolic enzymes. Source: Wiki.
Phase 2 – Conjugation
Phase 2 enzymes conjugate those phase 1 metabolites with glucuronide, sulfate, gluthathion, and other endogenous (=”belonging to the own organism”) hydrophilic molecules. These reactions result in phase 2 metabolites that are now water-soluble themselves and can be eliminated via the kidney. Also, in opposite to phase 1 metabolites, these products are mostly not able to exert toxic effects any more – i.e. the xenobiotic has been inactivated.
Compounds that are also susceptible for conjugation to acids of the bile can be excreted via the bile. But here, they might enter the so-called “enterohepatic circulation”. The bile is excreted to the intestine, where the gut microbiota might cleave the acids from the xenobiotics, making both again available for the uptake via the colon. This mechanism serves the purpose of saving valuable bilic salts, but as a side effect drastically increases the dwell time of xenobiotics that enter the circulation.
The “first pass” effect
This effect takes place when the metabolism of a xenobiotic is so quick that it’s fully metabolized with the first pass of the liver. Of consequence, only metabolites, but not the compound itself is found in the blood or any other organs.
Conclusion
Our body is detoxified from taken up foreign chemicals in 3 steps:
- enzymes of phase 1 metabolism add reactive groups to lipophilic compound, which results in still lipophilic, but more reactive phase 1 metabolites
- enzymes of phase 2 metabolism conjugate those products to gain hydrophilic products
- hydrophilic metabolites are excreted mainly via the kidneys (and the urine)
Outlook: metabolic activation and the impact of polymorphisms
As said before, this whole metabolic system serves as a defence. But seldom, a metabolite – and not the initially taken up compound – is toxic. Then, we talk about a “metabolic activation". Examples are the infamous mycotoxin aflatoxin B1, polyaromatic hydrocarbones or the chemotherapeutic drug irrinotecan.
Also, there are genetic variations (polymorphisms) among humans that lead to a different expression pattern of metabolic enzymes, which can manifest in a different reaction to one and the same toxin/drug by different people.
But all this will be addressed in following posts…after you now understand metabolism, I can write about that stuff. I hope you take the bait ;-)
Sources:
Book "Toxikologie für Naturwissenschaftler und Mediziner." Eisenbrandt, Metzler, Menneke. Wiley-VCH
A review
Wiki about the bile
Thank you for this post. I would give you 2 votes - but I can't, so you got re-steem.
In today's world of charlatans, it's really necessary to emphasize how the "detox" really works. It's done by organs, not by eating funny flowers, not by poking with the needles and not by filling "the wrong end" with obscure solutions.
Thank you once again
That resteem got him/her a new follower.
Thank you both.
him, and thank you!
thank you!
Don't me so mad against flowers. Some of them are good to add more taste to the food ;)
I'm a succulent guy :) Cactus is my favorite plant.
Ok, I lie, I have two Orchids as well...
cactus fruit are for sure part of some "detoxifying" cocktail^^
Nah, for real now: there are of course also natural occuring compounds that have proven beneficial effects on health. But I would never go so far as calling them "detoxifying"
The best detox fruit - pure black coal
that would be a great black-colored smoothie with proven detox-effects! u should patent the recipe.
DAILY DETOX:
Have a healthy liver and functioning CYP450 enzymes! Kidneys help, too!
This is totally a really helpful post especially for those of us trying to understand our bodies and rid ourselves effectively of toxins, I've been on medication for a while now and I know in the long run it could be harmful to my liver unless I at least put in some extra effort in detoxifying and getting rid of the harmful garbage, so far I'm doing all I can considering my should I say "financial" struggles, its a real upheel battle but I'm greatful to be alive, posts like yours enlighten the "needy" especially on how our system functions and how we can promote healthy and positive living through good life style choices and changing habits for the best.
Thanks for your post and I wish you a happy new year.
ty, happy to help ;-)
When it comes to science, you should always try and write like you're writing for a 5-year-old, I think! This was a bit heavy on undefined jargon, IMO.
ty for your input.
It is always a tradeoff between teaching the masses and staying scientifically correct. Sometimes it's hard to find the right balance. I wrote this post for the steemstem community, so I rather let the pendulum swing towards scientific correctness this time^^
@OriginalWorks
The @OriginalWorks bot has determined this post by @sco to be original material and upvoted it!
To call @OriginalWorks, simply reply to any post with @originalworks or !originalworks in your message!