Technique for gastric washing
The present medical technique deals with intestinal decontamination in circumstances where its indication and compliance is vital, such as poisoning by medicines or certain substances, which will be described later.
This method was first described and developed in 1812, and has been used for more than 200 years. It was most frequently applied around the 1970s with the use of tricyclic drugs.
Currently, with medical progress, this technique has fallen into disuse, due to the use of other modalities, such as the use of activated carbon, total intestinal irrigation, among others, which have shown greater effectiveness and fewer adverse effects.
Gastric lavage is still the form of intestinal decontamination of choice in some situations, especially those acute cases or where there is no antidote to the ingested substance. If performed correctly and at the right time, it can significantly reduce the amount of substance ingested and available in the gastric chamber and thus reduce the total dose of absorption.
This medical method has demonstrated great benefits if carried out early in the first to second hour of the ingestion of the toxic substance, especially those cases where there is an antidote and with a high mortality rate.
Its efficacy and effect diminishes over time, since such toxins can trigger a delay in emptying, while others can form masses or clusters in the stomach.
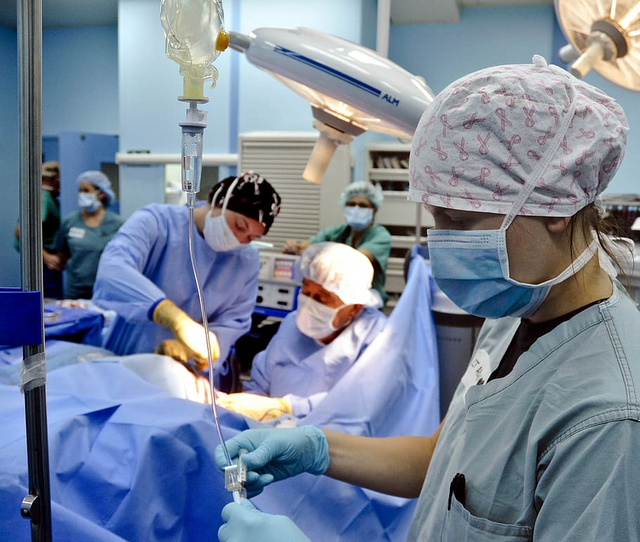
Public domain piqsels
Anatomy
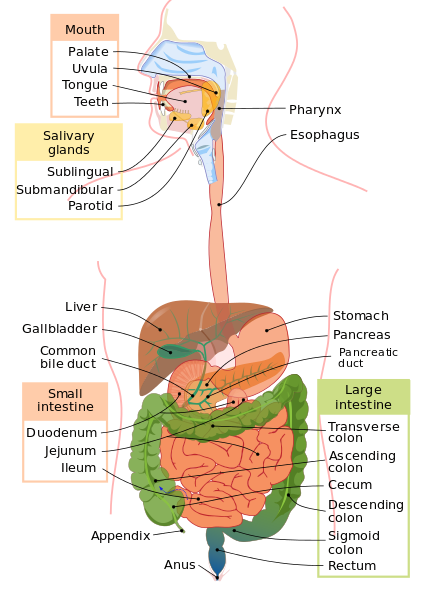
To reach the gastric chamber, it is necessary to know essential structures such as the oropharyngeal cavity, esophagus, and finally the stomach.
The esophagus is the muscular tube that extends from the pharynx to the stomach, it forms part of the digestive tube, and its function is to allow the passage of food.Stomach, muscular chamber, located between the esophagus and the intestine, which has glands that secrete gastric juice, which intervene in the degradation and digestion of food.
During gastric washing, it is recommended that the orogastric route be used instead of the nasogastric route. In the latter, nasal mucosa, turbinates and even the septum may be injured. The size of the tube to be used in these cases should be adequate. It is suggested that it be of medium to large size, which facilitates washing.

Public domain
Indications
Gastric lavage is indicated when we need to empty the stomach immediately, between the first and second hour, after an overdose or oral intoxication, as long as its use is not contraindicated.
However, other less invasive techniques should be evaluated, such as the use of activated charcoal or irrigation of the entire intestine.
The use of this technique should be considered when there is evidence or risk of significant toxicity, risk of death and absence of antidote.
There are special cases where gastric lavage is indicated as such:
Contraindications
An absolute contraindication to gastric lavage is severe cognitive impairment, with loss of protective airway reflexes, when the airway is not protected by other means. In this case the airway should first be secured by oro-tracheal intubation.
Flushing is contraindicated in cases of caustic ingestion, since it triggers mucosal damage which amplifies the risk of traumatic perforation during execution of the technique.
The presence of active, persistent vomiting, since it can eliminate the presence of the toxic in the stomach by itself and eliminate the need for lavage.
Gastric lavage cannot be carried out in the presence of foreign bodies in the digestive tract, due to the presence of anatomical malformations of the upper airway that prevent the passage of the gastric lavage tube.
It represents a relative contraindication in those cases of hydrocarbon intoxication, e.g. benzene, N-hexane, pesticides.
History of coagulopathy disorders, significant risk of bronchial aspiration during the procedure.
In neonates and infants, this procedure is contraindicated.
Materials required
Characteristics of the probe used for gastric washing
Most of them have a distal and a lateral hole. The semi-rigid ones are preferred to the soft ones or, in their absence, the flexible ones made of polyvinyl chloride.
It is recommended that several holes be made in the lateral area of the probe to improve suction, in case the probe has only one hole.
A larger diameter probe provides greater flexibility so that it is less likely to roll up, collapse or twist.
In the adult, a measurement of 30 to 50 french is preferred. In the adolescent, 30 to 34 french may be sufficient. In a young child, a 24-french tube may be used.
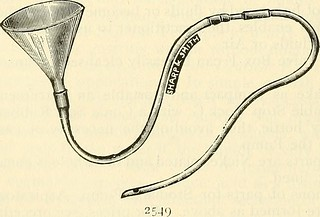
Gastric washing probe. Public domain Flickr
Preparing the patient
The patient or his/her representative must be informed of the procedure to be performed and informed consent must be obtained.
Initially, it is recommended that the patient be placed in a left lateral position and with 15 to 20º of Trendelenburg. The supine position is associated with a greater risk of bronchial aspiration.
Technique
The first step is to determine the length of the nasogastric tube to be inserted, which is taken from the xiphoid appendix to the tip of the nose and then brought to the earlobe. The distance taken on the tube should be labeled with a piece of tape.
It is recommended that the distal end of the catheter be generously lubricated and a mouth opener placed in the patient's oral cavity, or an oropharyngeal cannula, may prevent an uncooperative patient from biting the catheter.
Gently insert a washcloth into the patient's mouth and direct it to the hypopharynx.
Flexing the patient's neck makes it easier to pass the catheter.
Before infusing any type of liquid through the tube, it must be confirmed whether it is intragastric, and this is confirmed by aspiration of gastric contents or by auscultation of air insufflation over the epigastrium.
Once the correct placement of the tube has been confirmed, washing is carried out.
The first thing to do is to administer saline (saline or distilled water) at a dose of 10 ml or 15 ml per 1 kg with a maximum of 300 ml of the washing solution.
These fluid volumes can be administered with a funnel or a syringe through the free end of the tube. After a short period of 2 minutes, the liquid must be eliminated or extracted, either by gravity or by means of the syringe, and it is recommended to repeat the procedure 3 times or at least until no traces of the swallowed toxic material are evident.
Care after gastric washing
Most of these patients who present intoxication by some substance the first hours after washing must monitor the complications that may be triggered by that substance.
Monitor possible complications secondary to gastric lavage, such as esophageal perforation, among others.
Complications
Arrhythmias, hydroelectrolyte imbalance, gastric, esophageal or sinus puncture, pulmonary bronchoaspiration, pneumothorax, empyema, laryngospasm and oral or pharyngeal nasal lesions.
Gastric washing with activated charcoal administration
This technique has been documented since the time of Hippocrates.
Charcoal is obtained by distilling the substances obtained from the pyrolysis of vegetable matter or wood. It has the ability to adsorb toxins directly by their chemical properties thus preventing them from being absorbed into the gastrointestinal tract.

Activated charcoal in various forms. CC BY-SA 3.0
Activated carbon cannot be absorbed by the digestive tract, which allows it to pass through and be eliminated through the anus with the feces.
Indications
Activated charcoal is effective for most ingested toxic substances and is considered the method of choice for decontamination of the intestine. Its use is considered favorable for drugs that are metabolized in the liver and eliminated by bile.
Charcoal is safe and effective to such an extent that its use during pregnancy, lactation and in children is approved.
Contraindications
The only absolute contraindication is the presence of an unprotected area. The patient should be aware of the swallowing reflex at the time of the gastric washing with activated charcoal, or else the patient should be intubated and then the technique is performed.
This method is not effective against intoxication with lithium, iron, acids, heavy metal alkalis, cyanide, boric acid and alcohols.
Ingestion of caustic is a relative contraindication as coal is minimally effective in these cases, but if the caustic is combined with another substance that is absorbable by the coal, washing with it may be considered.
Technique
Coal should be administered as soon as possible, with emphasis on execution in the first two hours. It is preferable to use a watery paste in its presentation rather than a powder or capsule.
With a dose of approximately 50 to 100 gr in the adult 0 1 gr per kilogram of weight in the child with a maximum of 50 gr.The use of a nasogastric tube is recommended if the patient refuses to take the charcoal, the tube should have an estimated size of 16 french. Correct placement of the nasogastric tube is essential, and we must confirm its location prior to performing the lavage (already described).
It must be taken into account to minimize the pressure inside the gastric cavity, since if this is high, the risk of bronchial aspiration increases. For this reason, the administration of activated charcoal must be suspended four hours before removing the nasogastric tube.
The substances that tend to have the greatest response to the charcoal lavage are phenobarbital, theophylline, dapsone, diazepam, amitriptyline, carbamazepine, phenytoin, quinine, salicylates, piroxicam, digoxin, and tricyclic antidepressants.
Complications
The most dangerous and frequent if this technique is not correctly exercised is bronchoaspiration, triggering a severe pneumonitis that can compromise the ventilatory pattern, causing it to collapse and finally death.
Other complications after bronchoaspiration are the formation of empyema and bronchiolitis obliterans.
Intestinal obstruction is a rare and infrequent complication that may be accompanied by abdominal perforation, which may require immediate surgical intervention.
Sources:

steemSTEM is a project of the chain of blocks that supports the scientific content in different areas of science. If you want to know more about this wonderful project you can join the server in discord
This article will be published at https://www.steemstem.io/

link
If you have any questions about any topic of medicine or present any disease you can comment the publication or write me in discord and I will attend you.
Dr. Ana EstradaI hope you enjoyed my content.
I remember one time my dog took rat poison. What we came up with on the recommendation of the neighbors was to give him milk. In the end my dog lived a few more years.
I guess this method is for large amounts or some stronger toxic elements.
This post has been voted on by the SteemSTEM curation team and voting trail. It is elligible for support from @curie and @minnowbooster.
If you appreciate the work we are doing, then consider supporting our witness @stem.witness. Additional witness support to the curie witness would be appreciated as well.
For additional information please join us on the SteemSTEM discord and to get to know the rest of the community!
Thanks for having used the steemstem.io app and included @steemstem in the list of beneficiaries of this post. This granted you a stronger support from SteemSTEM.