Facts About Ovarian Cysts
What is a Cyst?
A cyst is simply a collection of fluid, similar to a water filled balloon.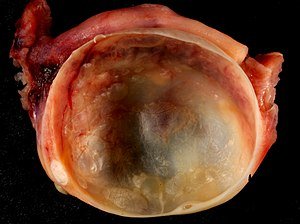
Functional Cysts
Functional cysts are the result of a glitch in the normal process of ovulation. They are called functional because they arise during normal ovarian processes. They rarely exceed five to six centimeters in diameter.
Follicular cysts develop from egg follicles in which the egg fails to mature. Fluid collects in the egg follicle, forming the cyst. The majority of follicular cysts dissolve without any treatment, and they seldom become larger than five centimeters. They may rupture and cause pain, but it most often resolves quickly and only needs to be treated with analgesics. They are not cancerous, and they are unlikely to recur. Women who do have recurrent problems may benefit from hormone suppression of the ovary, usually with birth control pills.
Corpus luteum cysts develop from mature egg follicles. The name is derived from the yellow coloration the tissue receives from the hormone changes associated with ovulation and means "yellow body." Corpus luteum cysts are usually small, and it is common to have a small amount of bleeding and leakage of fluid from the corpus luteum when the egg is actually released from the ovary. This may produce pain referred to as mittelschmerz.The pain is usually brief and not severe. Occasionally, a larger cysts forms and ruptures, with more pain. Corpus luteum cysts also usually resolve without treatment.
Although some functional cysts may produce enough internal bleeding when they rupture to require surgery, this is uncommon. The combination of the patient's history and findings on ultrasound help make the diagnosis. All that is needed for cysts smaller than five to six centimeters is usually medication for pain relief and observation. Ruptured cysts will no longer be visible on ultrasound, because they collapse when the enclosed fluid spills out, but the fluid may be seen as a puddle behind the uterus.
Other Common Benign Cysts
Dermoids (teratomas) and endometriomas are also common.
Dermoids arise from egg cells which, though unfertilized, produce various tissues, such as skin and hair and sometimes even teeth. Most are noncancerous, but they do need to be removed. Dermoids are often without symptoms, but they do have a propensity to cause torsion, or twisting, of the ovary around its supporting structures. Sometimes they can grow very large, though cancerous teratomas are not common.
Endometriomas develop from tissue similar to that lining the uterus. There may be implants of such tissue (endometriosis) elsewhere in the pelvis. The endometriosis bleeds cyclically in association with the menstrual period and can produce ovarian cysts filled with old blood that looks like milk chocolate, the endometrioma or "chocolate cyst." Menstrual pain can be severe. Endometriosis is associated with infertility and is sometimes found in women who are having problems with conceiving even if they do not have pain. Endometriosis can be treated with surgery, medications, or both; however, removal is often recommended for endometriomas.
Cystic Tumors
Cystic tumors, the most common of which are cystadenomas, often have a typical appearance on ultrasound. Because of the possibility of cancer, additional testing may be needed. Cystadenomas may have septations, or subdivisions within the main cyst. They, too, can grow to large sizes and need to be removed. Removal is the only way to determine if the cyst is cancerous.
Ovarian cancers are more common in older women. Since postmenopausal women do not ovulate, even smaller cysts may be cancerous. Careful observation and additional diagnostic tests are essential.
When a Cyst is Diagnosed
Premenopausal women with functional cysts need not be alarmed. Though they may cause pain, the risk of cancer is low and the likelihood that surgery will be needed is small. Even small cysts in postmenopausal women, who do not ovulate and do not form functional cysts, need careful evaluation.
Larger cysts in all age groups may need further testing, but the possibility of cancer is small. The gynecologist should be willing to explain the test results and outline the best way to proceed.