HIV-Infected Needle Attacks Be Carefull Friends..

HIV infected needles found in public take only 2
minutes of your time to save your life:-
When getting a HIV- infected needle by accident, calm down and follow these steps:
- Go to the nearest house for soap, use it to sterilize the wound, then rinse.
- Within 24 hours, go to medical facility to buy anti-HIV medication. Note that the drug only works within 72 hours, taken continuously for 4 weeks.
For the sake of yourself and the community, please take a couple of seconds of your time and share this message with all your friends!

Recently, a girl who went to the movies, sat down in one of the theater seats, and felt a stabbing pain. She quickly stood up and found the needle of a medical syringe sticking out of the seat. There was also a note that said, “You have been infected with HIV”.
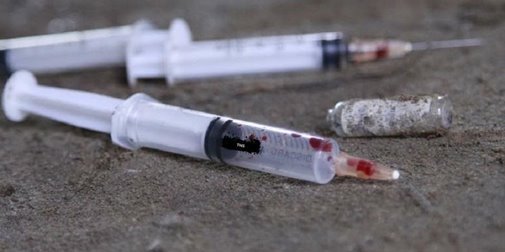
The Centers for Disease Control reports that similar events have taken place in several other cities recently. All of the needles tested HAVE been positive for HIV. The CDC also reports that needles have been found in the coin return areas of pay phones and soda machines.
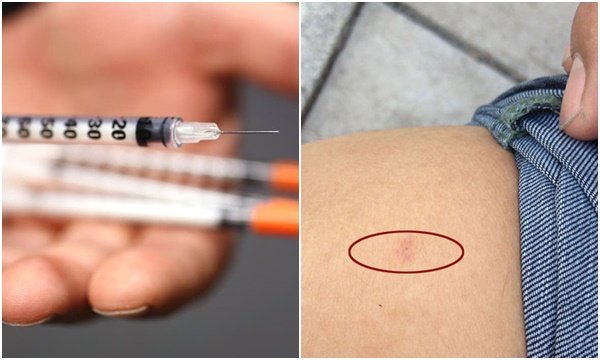
Another girl preparing to marry in the next few months was stabbed while watching the movie. Although the doctor said it took six months for the virus to be strong enough to destroy the immune system and one healthy patient could live five to six years, the girl died in the fourth month because of shocking.

Be careful the next time you go to a cinema. These people could be anywhere!! An experience of a friend of my brother’s wife left me speechless. Please do send this out to everyone you know. This incident occurred in Bombay’s Metro cinema (Among the best in town).
They were a group of 6-7 College girls & they went to the theater to see a movie. During the show one of the girls felt a slight pinprick but did not pay much attention to it. After sometime that place began to itch. So she scratched herself and then saw a bit of blood on her hands. She assumed that she had caused it. At the end of the show, her friend noticed a sticker on her dress and read the caption. It read “Welcome to the world of AIDS”. She tried to pass it off as a practical joke but when she went for a blood test a couple of weeks later (just to be sure), she found herself HIV Positive.
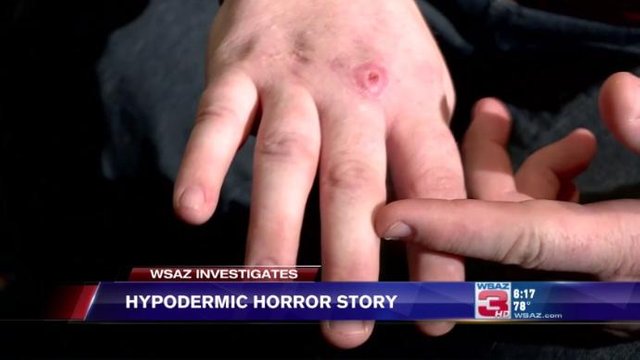
When she complained to the cops, they mentioned that her story was one of the many such cases they had received. It seems the operator uses a syringe to transfer a bit of his/her infected blood to the person sitting ahead of him/her. A horrible experience for the victim as also the family & friends. The WORST bit is that the person who does it gains NOTHING where as the victim loses EVERYTHING.
So, be careful . . .
PLEASE CHECK YOUR CHAIRS WHEN GOING TO THE MOVIE THEATRES!!!!
An incident occured when a friend’s co-worker went to sit in a chair and something was poking her. She then got up and found that it was a needle with a little note at the end. It said, “Welcome to the real world, you’re “HIV POSITIVE”.
Doctors tested the needle and it was HIV POSITIVE. We don’t know which theatre this happened at, but it happened in Hawaii.
“BE CAUTIOUS WHEN GOING TO THE MOVIES!”
IF YOU MUST GO TO THE MOVIES, PLEASE, PLEASE CHECK!!!!! One of the safest way is NOT sticking your hands between the seats, but moving the seat part way up and down a few times and REALLY LOOK!!!!!!! Most of us just plop down into the seats.
PLEASE READ THIS CAREFULLY! IT MIGHT SAFE YOUR LIFE!
This is happening in Montreal. A couple of weeks ago, in a movie theater, a person sat on something sharp in one of the seats. When she stood up to see what it was, a needle was found poking through the seat with an attached note saying, “You have been infected with HIV.” The Centers for Disease Control reports similar events have taken place in several other cities recently. All of the needles tested HAVE been positive for HIV. The CDC also reports that needles have been found in the coin return areas of pay phones and soda machines. Everyone is asked to use extreme caution when confronted with these types of situations. All public chairs should be thoroughly but safely inspected prior to any use. A thorough visual inspection is considered a bare minimum. Furthermore, they ask that everyone notify their family members and friends of the potential dangers, as well. Thank you.
The previous information was sent from the Regina City Police Department to all of the local governments in the Saskatchewan area and was interdepartmentally dispersed. We were asked to pass this to as many people as possible. This is very important! Just think you could save somebody’s life, just by passing this on. Please take a Couple of seconds of your time and pass this on. Thank you for your precious time and consideration!

That stops public health workers from trying exchanges and other programs that could curb infection rates and increase access to information about addiction treatment.
"There’s a lot of things we can do from a preventative standpoint and the biggest hindrance right now is that it’s illegal," said Bartholomew, who works at a needle exchange program at the University of Miami. "If you possess a syringe, you can be prosecuted for it. And if you distribute a syringe, you can be prosecuted for it as well."
Lawmakers have yet to act on a needle exchange bill in Harrisburg has even as the state grapples with an increasing and above-average rate of opioid overdoses, at 18.5 deaths per 100,000 residents in 2016, according to the National Institute on Drug Abuse.
Generational Forgetting
Infection rates among county residents age 13-24 have climbed, MacDonald said, including within Latino neighborhoods. National data show a rise among young people too. National Institutes of Health researchers have observed what they label “generational forgetting.” Young people may be less likely to perceive the dangers of HIV infection than are older people, especially older populations within the LGBTQ community, who witnessed their friends die in the blistering AIDS epidemic of the 1990s.
According to the U.S. National Institute on Drug Abuse, in 2015, people aged 13-24 comprised only 16 percent of the population, but 22 percent of new HIV diagnoses.
Young gay and bisexual men accounted for 84 percent of all new diagnoses for ages 13-24. People too young to remember do not comprehend how deadly AIDS was. The “generational forgetting” theory aligns with county data.
Intensity of stigma
“There is significant stigma attached to seeking help, and especially in seeking help from a government agency, which is what the county health department is,” MacDonald explained. And without private hospitals and doctors offering information, county facilities are the only option. “We are trying to work with regional hospitals to increase the number that will offer testing,” he said.
MacDonald notes that a number of new diagnoses are coming from private clinics such as Planned Parenthood and Clinicas del Camino Real, which is a bicultural and bilingual medical clinic that serves those with limited income and resources.
“There is a huge population in Oxnard that we are not reaching,” MacDonald says. “There is a huge youth population, as borne out by the increase in numbers of people 35 and under.”
Even when there is no threat of HIV specifically, youths tend not to be vigilant: “Teens are infamous for incorrect and inconsistent use of condoms,” Dr. ChrisAnna Mink, a Carson, California, pediatrician, recently wrote in an article addressing rising levels of sexually transmitted disease among teens.
Few testing locations
“Diversity Collective is responding, through our HIV/AIDS Education and Prevention program,” MacDonald said. “There was that spike, with 84 new cases, in Ventura County in January 2017. What it showed was two new trends. The largest population of infected people were age 35 and under. There was also an increase in ages 55 and older.”
Pinpointing a reason for an increase in ages 55 and older is not easily accomplished by any one factor, but MacDonald notes that over the years, there have been few resources for getting HIV-tested. “There was only the Ventura County Health Care Agency and us — Diversity Collective — working on this. The recent data was welcomed by Diversity Collective, as it pointed to more people being tested,” he said.
Expansion possibilities might include HIV testing during routine blood tests done at hospitals and emergency rooms. Patients can currently opt out of this if they do not want it included in their medical tests, but if it became routine, the number of county cases might more accurately reflect infection rates. When people coming to an emergency room for blood work agree to be tested for HIV as well as their other concerns, countywide data could become more accurate. “We need to be pushing education and information,” MacDonald said. “We’d like to see HIV testing included by doctors’ offices as a part of normal blood work, because we know that is not taking place now.”
Online dating and hookup websites
County rates of infection are similar to rates that are climbing nationwide. Many experts have pointed to hookup sites used primarily by men seeking men — or MSM — for sex, as the reason.
MacDonald does not agree that hookup sites are a prime reason. “There are organizations that want to point to online hookup sites. I don’t see it that way,” he said. “These sites, such as Grindr, have been around for 10 years. So use of these sites does not completely explain the increase.”
According to the Centers for Disease Control, 15 percent of infected gay men do not know that they are infected, which contributes to risk if they use hookup sites for unprotected sex. This is what happened in the 1980s. No one knew they were infected, so they did not use condom protection, thus spreading infection with great speed.
On March 26, MSM hookup site Grindr.com, which claims 3.3 million daily users worldwide, for the first time and following public criticism, started displaying reminders about frequent HIV testing on the site, along with directions to nearby testing locations. The world’s largest provider of gay dating phone apps, Grindr.com’s announcement also stated thatthe site will allow clinics, gay community centers and other testing sites to advertise for free.
This decision was made to “reduce H.I.V. transmission and support our whole community — regardless of H.I.V. status — in living long and fulfilling lives,” Jack Harrison-Quintana, Grindr’s director for equality, told The New York Times. Several experts cited in the Times article greeted the news positively. Is there evidence that HIV infection increases within the MSM community because of hookup sites? Dr. Jonathan Mermin, chief of AIDS and Sexually Transmitted Diseases at the Centers for Disease Control and Prevention, said that CDC data show many men who use hookup websites to find other men nearby seeking sex are at high risk of getting infected.
Phone apps can ease accessibility to both responsible, or risky, behaviors. “Men who have sex with men, or MSM, no longer have to go to bars to meet,” Ornelas pointed out. For MSM who are not comfortable approaching other MSM, there is the ability to hide behind an app, and contact someone anonymously. “This is true, for example, if you’ve never dated men, or have only been in heterosexual relationships; here’s an easy way to connect with men seeking men.
“Some LGBTQ advocates do not like making sites like Grindr the villain,” Ornelas notes. He said responsibility should ultimately fall on the visitor to the site or app. “A lot of people are against vilifying these apps. Interestingly, sexually transmitted diseases, or STDs, including chlamydia, gonorrhea and syphilis, are rising, and few observers are vilifying sites like match.com or eHarmony.com the way Grindr has been.”
No safe place to go for help
Diversity Collective this year opened a community center to serve LGBT patients who have had no other place to go. VCPH facilities offer free HIV testing Monday through Friday.
“We always knew the numbers were bigger than what we know. In the past, the estimate was that 2,000 people in the county had HIV,” MacDonald said. “But the Ventura County Health Care Agency was offering testing and treatment, and only seeing 400 people. So you had to ask, where are all the others?”
Inadequate prevention
Another contributing factor may have been inadequate health-care-provider collaboration toward prevention. For example, pre-exposure prophylaxis pills, called PrEP pills, provide a way for people who are HIV-negative and sexually active to prevent HIV infection by taking a pill every day. “These are pills people can take before having sex, which are somewhat like birth-control pills, and there are also morning-after pills, although the morning-after pills do have serious side effects,” MacDonald said. “But we have observed that about 30 percent of county providers are not familiar with PrEP pills. So when people see a local doctor, for example, for an annual checkup, their doctors may not inform them about PrEP pills, as some doctors do not know about them. A number of local hospitals are not informing patients about PrEP pills either, so people are not receiving information.”
Deportation qualms
Undocumented people do not tend to seek out health care, and if they become infected due to any of the other factors, they may not get tested, and can therefore spread infection. “One factor is that within the current political climate, undocumented people are afraid to seek health care — in this county in particular, it’s really important,” Donaldson said. “Current immigration policies really harm public health.”
Moving forward
VCPH’s HIV/AIDS Center operates a needle-exchange program, also called a syringe replacement program, which can significantly decrease the spread of infection. “Research solidly backs that up,” Donaldson said. “Research shows rates of transmission of blood-borne infections, including HIV and hepatitis, decrease with needle-exchange programs. Needle exchanges bring significant harm reduction to communities,” he said. “In terms of promoting and maintaining general public health, harm reduction is always a good thing.”

The county Syringe Replacement Program allows drug users to trade in their used syringes for new ones. This is a countywide effort to slow or stop the spread of HIV caused by infected needles. Returning used needles to county facilities keeps them, off the street, out of lawns and out of trash bins, thereby keeping nonusers out of harm’s way.
“I think we have also reduced related emergency room and hospital visits for our participants,” Ornelas said. The exchange program results in a decrease in infections and abscesses, once participants are using clean needles and safer injection supplies.
“Program participants come from a variety of situations and different socioeconomic levels: we have some who live with their families and hold down regular jobs, some who are homeless, and the rest fall somewhere in the middle,” Ornelas said.
The main thing is to insure that participants have a clean syringe for every injection. That is the goal. “We are trying to stop the spread of infection and increase harm reduction,” Ornelas said. “We explain to participants that if we give them 30 needles, for example, to last a week, we hope to see 30 used needles returned the following week, but this does not always happen.
“We give participants sharps containers to safely store used needles until they can be returned to us,” Ornelas explained. This is done so that there is little excuse for not returning them. Different sizes of containers are offered, which cannot be legally deemed to be drug paraphernalia.
To prevent stray, used needles from being found and picked up on the street, the program does aim to get all needles that are given out to be returned. “Along with a list of our other SRPs and the days they operate, we give participants a list of other places where they can return the needles,” Ornelas said. “Clinics and facilities located throughout the county that also accept used syringes might be located closer to where participants live and are open on days their closest SRP is closed.”
“In 2016 we gave out 40,192 syringes. We took in 41,064 syringes,” Ornelas said. Also in 2016, the program resulted in 2,753 encounters with participants, including visits by both repeating and one-time participants.
In 2017 103,914 syringes were given out and 83,560 syringes were taken in. Total 2017 encounters were 3,287, which was an increase of 534 encounters over 2016. “Letting the public know what we do offer is key,” Ornelas says. “And getting the message out.” (Ventura County has about 850,600 residents total.)
The program also distributes Overdose Rescue Kits, known as NARCAN Kits, to those who use opiates such as heroin. Kits and training to administer them are also available to those who live with opiate users. They are commonly called “NO OD” kits. “In 2016, we distributed 125 kits, and we had 35 total overdoses prevented with these kits,” Ornelas said. “In 2017, we gave out 327 NARCAN kits, and had 88 overdoses prevented, as reported to us,” he said.
VCPH operates SRPs once a week in Simi Valley, Oxnard, Ventura and Santa Paula. An SRP test run is being performed at the Health Care for the Homeless’ One Stop program at the River Haven transitional living program. While there aren’t many inhabitants in the River Haven huts, there are an estimated 100 or more living in the river bottom right behind it. Used syringes have been found there frequently, Ornelas said.
Keeping the issue ‘in front of people’s faces’
“There hasn’t been anyone to keep the problem in front of people’s faces,” Coffman-Gray said. “Publicity about PrEP is an example. If you don’t know about it, you are not going to use it.
“The rising rates are almost all MSM, or women who have sex with MSM,” he said. “Surprisingly, about 27 percent were over age 50. About 49 percent were Caucasian and 48 percent were Latino.
“I believe drugs are involved because they lower inhibitions,” Coffman-Grey noted. But he agrees that many people are still hiding “in the closet” because stigma is so powerful. He sees evidence that many in the Latino community do not want to ask questions about treatment because they do not want to be perceived as being gay.
Hookup sites are “certainly exacerbating,” Coffman-Grey said, but an equally compelling factor is lack of community centers, because that’s been a problem since before 2012. “There has not been a community resource center for years,” Coffman-Grey said. “There were so many people with no place to go.
“People were so scared in the 1990s,” Coffman-Grey recalled. “It was a time of such intensity and hatred. People with AIDS or HIV could find no place to rent or live. No matter how much money we had to offer, landlords would not rent to AIDS patients. Dying patients were rejected by their families. Imagine, to be dying in droves, rejected by their families and having no place to live. People were literally kicked to the curb. I was involved then, and we could not find anyplace to house people.”
“We just have to keep on it,” Coffman-Grey said. “We have to keep educating people, and keep raising awareness. People are still dying of this disease. We need to let people know you can still die of this.”
Donaldson notes: “My main message is, get informed, be safe and get tested.”
House Bill 196 would allow authorized agencies to provide syringes, needles and other items to drug users through an exchange program. Agencies also would provide information about addiction treatment. It was introduced last year by Rep. Ed Gainey, a Pittsburgh Democrat.
The bill would redefine “drug paraphernalia” to exempt needle and syringe exchange programs.
“As the law does not permit needle and syringe exchanges, many other communities that could benefit from these exchange programs are opting not to do them in order to follow the law,” Gainey wrote in a memo about the bill. “Some exchange programs that operate in other cities do so in fear of being arrested.”
The bill was referred to the House Health Committee in February 2017. It’s still there.
In Pennsylvania, 11.7 percent of new HIV infections in women and 8.4 percent in men were attributed to injection drug use in 2015, according to the National Institute on Drug Abuse. About 27 percent of people living with HIV in the state contracted it through injection drug use.
TAHLEQUAH, Okla. (AP) — Cherokee Nation officials in Oklahoma say more than 180 patients affected by a tribal hospital nurse improperly reusing syringes have been notified they can receive free blood tests and that no one has tested positive for HIV or hepatitis.
So far, 127 of the patients have been tested. Tribal officials said Thursday it's unclear whether the rest will get tested.
Experts have said the chance of infection is remote. The hospital CEO said patients were never directly in contact with a needle.
Officials said the nurse violated protocols by using the same vial of medication and syringe to inject multiple intravenous bags at W.W. Hastings Hospital in Tahlequah. The nurse no longer works for the tribe.
CDC says more routine HIV screening would reduce new infections
Clinicians aren't offering HIV testing to many people unaware they are infected with the virus. More routine testing and digital tools to help remind clinicians would go a long way toward treating infected patients and ending stigmas and barriers to care, according to public health experts.
"Clinicians who have a routine way to assess sexual risk are more likely to offer HIV testing," said Cyprian Wejnert, an epidemiologist with the Centers for Disease Control and Prevention's Division of HIV/AIDS Prevention. "However, we need to make the process easier."
Wejnert was lead author of a report published Tuesday in JAMA that found approximately half of individuals at higher risk for contracting HIV—such as men who have sex with men and people who inject drugs—were not tested for the virus in the past year and said they were not offered testing by clinicians during routine visits.
An estimated 15% of people living with HIV did not know they were infected, according to the study, but they accounted for about 40% of new HIV transmissions in the U.S. every year. The overall number of new HIV infections in the U.S. has fallen for the past several years, from 41,800 in 2010 to 38,500 in 2015, according to the CDC.
But the opioid epidemic has brought about new cases. Injection drug useaccounted for 40% of all new HIV infections in 1990, but fell to make up just 6% of cases by 2015. In 2015, however, cases began to slightly increase for the first time in two decades, going from 2,392 cases in 2014 to 2,635 in 2015. A large contributor to the increase was the HIV outbreak that occurred from late 2014 to early 2015 in Scott County, Ind.,where most of the 181 people who contracted HIV did so through sharing infected needles.
Separately, young gay and bisexual men accounted for 81% of all new HIV diagnoses in people aged 13 to 24 in 2016, with young black gay and bisexual men among the most severely affected groups.
Since 2006, the CDC has suggested clinicians routinely screen all people age 13 to 64 and to test those at higher risk every year. But a recent CDC studyfound only little more than a third of U.S. adults tested for HIV between 2006 and 2016. Those who had been tested waited three years between tests. Among higher-risk individuals, only 62% were ever tested for HIV, with the median interval since their last test being 512 days, or nearly a year-and-a-half.
Clinicians say patients worry positive diagnoses might lead them to be ostracized by their family and friends.
Dr. Margaret Hoffman-Terry, an HIV specialist at Lehigh Valley Hospital in Allentown, Pa., and board chair at the American Academy of HIV Medicine, said the CDC guidelines call for adults to be tested at least once, only to get tested again based on their amount of risk.
"Time and time again studies show that providers are very bad at predicting risk," Hoffman-Terry said. "And patients often don't disclose." She said the recommendations should reflect the importance of making HIV testing a more regular clinical practice and that alerts prompting clinicians to test for HIV should be part of a hospital's electronic health record system, the same way hepatitis C is currently handled.
"The most effective strategies toward increasing testing are those that do not place additional demands on clinicians or patients and can be seamlessly integrated within the normal clinical workflow," Wejnert said.
The first part is proven to be FALSE and the second part is just blatant plagiarism.
@steemflagrewards - Flag for Plagiarism.
(and perpetuating proven-to-be-false-claims)
Steem Flag Rewards mention comment has been approved! Thank you for reporting this abuse, @serylt categorized as plagiarism. This post was submitted via our Discord Community channel. Check us out on the following link!
SFR Discord