Blue People in Kentucky: The True Story of the Fugate Family with Blue Skin
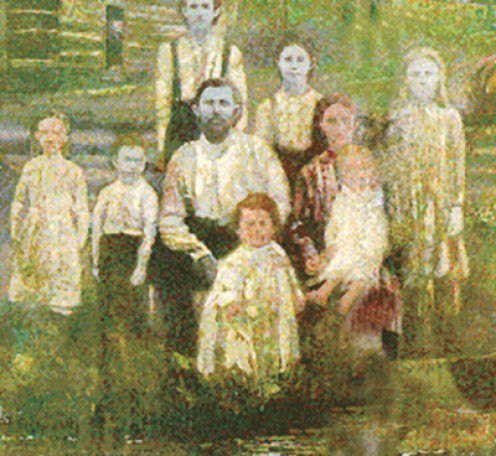
A (Healthy) Blue Baby
“Have you ever heard of the Fugates of Troublesome Creek?”
This simple question by a knowing grandmother solved a riddle for a little boy born blue.
When little Benjamin “Benjy” Stacy was born in a small hospital near Hazard, Kentucky, he was the picture of health. He was also very, very blue. So blue, in fact, that his skin was the deep purple color of a plum. His doctors were alarmed by the child’s color, and immediately sent him by ambulance to a hospital in Lexington, Kentucky.
Little Benjamin was subjected to an enormous variety of tests in an attempt to explain the startling blue color. While he did not appear to be in any distress, doctors began to set up a blood transfusion for the tiny baby. That was when his grandmother decided to speak up:The boy’s father explained that his paternal grandmother Luna was also blue – and apparently was quite healthy in life.
Benjy’s blue color started to fade a bit over the next few weeks, and as he grew the only remaining traces of blue coloration were in his lips and nails – the color was particularly noticeable when he became cold. The doctors came to the conclusion that Benjy had inherited a rare gene found in the Appalachians – a gene which turned entire generations of one family blue.
French Orphan Martin Fugate: The First Blue Man in Kentucky
In 1820, Martin Fugate and his wife Elizabeth Smith moved onto the banks of Troublesome Creek, a beautiful area in Appalachian Kentucky. There is no official recording as to whether Martin was actually blue, but he and his wife both carried a recessive gene that would turn their son Zachariah Fugate a startling blue color. Martin and Elizabeth had seven children: four of them were blue. Since the gene causing the blue coloration is recessive, the family had a 25% chance of having a blue child with each pregnancy if Martin and Elizabeth were carriers. If Martin was blue, the odds would have increased to 50% for each child, as Martin would have carried two copies of the recessive gene.
Since the Appalachian region was rural and isolated, inter-marriages occurred. Fugate descendents married other Fugate descendents, concentrating the “blue gene” over the generations.
Luna Fugate, little Benjy’s great-grandmother, was one of the bluest Fugates known to the Appalachian region. Luna was described as being blue all over, with lips the color of a dark bruise. Although blue, she was entirely healthy, and had 13 children in her 84 year span of life.
The blood on the left has a bluish tinge, due to excess amounts of methemoglobin. The blood on the right is normal.
The blood on the left has a bluish tinge, due to excess amounts of methemoglobin. The blood on the right is normal. | Source
What Caused the Blue Skin Color?
Scientists, of course, were quite intrigued as to the cause of the blue skin tone among the Fugate family. In the 1960’s, a young hematologist named Madison Cawein traveled to the region, with an aim to cure the blue people of their skin color. The doctor hiked through the Appalachian hills, on a mission to find the famous blue people of Kentucky.
He finally found a family willing to participate in her study of the condition, and ruled out any heart or lung condition as the cause of the blue skin. Apart from being blue, the people were entirely healthy.
Dr. Cawein began to suspect a rare condition which causes a blue form of hemoglobin to circulate in the blood. The condition is called methemoglobinemia, which is caused by large circulating amounts of methemoglobin – the methemoglobin is not harmful, but large amounts of the non-functional hemoglobin will tint any tissue containing a blood supply blue.
The first family to volunteer for research, Patrick and Rachel Ritchie, did not want to be blue. Dr. Cawein did several tests to find the cause of the methemoglobinemia, and found the Fugate family was missing an enzyme called diaphorase, an enzyme that converts the methemoglobin back into functional hemoglobin. As the Fugate family’s methemoglobin could not be reconverted into the normal hemoglobin molecule, the blue methemoglobin began to build up and become very obvious in the pale skin of the affected family members.
An Ironic Cure for Blue Skin
One way to convert blue methemoglobin back into red hemoglobin is to use a dye called methylene blue. Ironically, a blue dye could change the blue color of the affected blood into a normal red color. Ascorbic acid is another method of treating the condition.
Of course, it was a tad difficult to convince the blue people of Kentucky that a blue dye would cure the condition: Patrick and Rachel volunteered to try the treatment.
A simple injection of the dye caused a stunning color change: within minute, Patrick had gone from blue to pink. Having found a way to cure the blue skin color, Dr. Cawein left the people with a supply of methylene blue pills – the pills must be taken on a continual basis, since the body eliminates the dye on a regular basis.
Since the dye also tints the urine blue, some of the older mountain people thought the blue color of their skin was literally “pouring” out of them.
As coal trains and other modern highway connectors began connecting Troublesome Creek with the rest of the nation, people began leaving the area. The gene is no longer concentrated, and the chance of intermarriage between two gene carriers is remote. Still, the possibility does exist – as the parents of little Benjy Stacy proved.
The gene found in the Fugate family is from a line of French Huguenots, whose descendents settled into Kentucky, Ireland, and Finland.
Methylene Blue: it turns blue people
What Became of Benjy Stacy?
The little boy born blue has grown up. He attended Eastern Kentucky University, married, and lives a perfectly typical life in Fairbanks, Alaska. Other than an occasional worried comment from unknowing friends about the color of his lips or fingernails, there is little outward sign of the methemoglobinemia.
Types of Congenital Methemoglobinemia
One form of congenital methemoglobinemia is caused by a deficiency in NADH cytochrome b5 reductase. It has several types, which vary in severity of the symptoms:
Type I: This type is limited to the red blood cells, and causes a blue color.
Type II: The enzyme is deficient in all tissues, and devastating systemic effects are seen – mental retardation, a small head size, and other central nervous system problems are severe. The child will also present with a blue color.
Type III: The entire blood cell system is affected, including platelets, white blood cells, and red blood cells. Fortunately, this variant does not cause any medical problems (other than a blue skin color).
Type IV: This type only affects the red blood cells, and causes a chronic blue color. No other medical problems are associated with Type IV.
The majority of methemoglobinemia cases are caused by an acquired problem: the person has been exposed to oxidizing drugs, toxins, or chemicals. In the case of acquired methemoglobinemia, the patient must be monitored for low blood oxygen levels and anemia, as the amount of circulating normal hemoglobin may be reduced to extremely low levels.